- Trauma and Emergency Fracture
- Joint Replacement Centre
- Keyhole surgery of the joints
- Sports Medicine Centre
- Frozen Shoulder
- Neck and Lower Back Pain
- Paediatric Ortho care
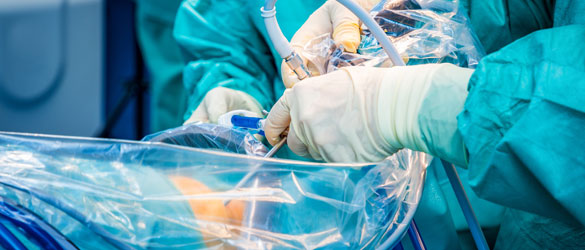
Trauma and Emergency Fracture

Orthopaedic injuries can be serious and traumatic, requiring immediate care and possibly surgery. At Kauvery Institute of Orthopaedics and Neurosciences, we provide expert care in the management of both simple and complex injuries to the musculoskeletal system. Our round-the-clock accident and trauma management services offer the highest level of all possible care to the seriously injured patients.
The Kauvery Institute Orthopaedic Accident and Trauma Care team of medical experts, includes trauma/acute care surgeons, neurosurgeons, vascular surgeons, plastic surgeons and other physicians who address traumatic injuries.
Regardless of the nature of trauma to your musculoskeletal system, at The Kauvery Institute of Orthopaedic and Neurosciences, our endeavour is to offer best of care, utilizing our collective, medical acumen, state of the art technology and international medication safety care to restore our patients’ quality of life.
- Injuries that impact part or parts of the musculoskeletal system in an accident
- Compound fractures of a complex nature to the hips and knees
- Shoulder, wrist, and elbow trauma management
- Minimally invasive fracture repairs
- Complications arising on account of trauma
- Ankle Sprain
- Shoulder dislocation
- Stress Fractures
- Meniscus Tear
- Tennis Elbow
- Plantar Fasciitis
- ACL Tear
- Rotator Cuff Tear
- Distal Radial Fracture
- Carpal Tunnel Syndrome
- Most advanced medical technology
- A constant upgrade of an array of diagnostic devices and orthopaedic instruments
Joint Replacement Centre
Joint replacement is a surgical procedure in which arthritic or damaged joint parts are removed and replaced with plastic, metal, or ceramic prostheses or devices that are designed to duplicate the movement of the joint as closely as the original joint.
Several types of conditions can cause joint pain or disability, consequently requiring a patient to consider joint replacement surgery.
When a patient is referred for a joint replacement program, the Orthopaedic Surgeon will suggest treatments based on the findings and diagnosis, taking into consideration, the age, activity levels, and medical history of the patient. The evaluations will be based on radiological, medical, physical, and historical records of the patient. Both non-surgical and surgical options will be considered and discussed by the orthopaedic surgeon as part of counselling and educating the patient.
Joint replacement is a surgical procedure in which arthritic or damaged joint parts are removed and replaced with plastic, metal, or ceramic prostheses or devices that are designed to duplicate the movement of the joint as closely as the original joint.
Once you have chosen to have your joint replaced, the orthopaedic surgeon will schedule the surgical procedure. The surgical team will administer anaesthesia, which could be either spinal or general. Once the anaesthesia takes effect, the surgical team will replace the damaged joint with a prosthesis.
The length of the surgery will depend on the extent of damage to the joint, and therefore, each surgery will be different, depending on whether there are other complications involved. Post-surgery, the patient will be held in a recovery room until such time that the anaesthetic effect has worn off.
After a knee or hip replacement surgery, the process to help you regain your mobility will begin, such as standing or walking. To start with, our trained and experienced physiotherapists will assist you in strengthening the muscles with gentle exercises, so that you can regain mobility. If the joint replacement was in your shoulder, generally you will be encouraged to begin exercising it on the very same day of the surgery.
Keyhole surgery of the joints
Keyhole surgery or Arthroscopy is normally performed through two very small puncture holes, where one hole is used to pass the arthroscopic instrument through and the other hole is used for the camera, which is used to visualize the joint.
An orthopaedic surgeon, with the help of an arthroscopic instrument, probes, diagnoses, and treats problems with joints. It is a procedure that is generally used on the shoulder, elbow, wrists, knees, and ankle joints. When a patient has joint problems, such as swelling or stiffness, an arthroscopy may be recommended by the orthopaedic surgeon, in the event the imaging tests have not revealed the crux of the swelling or stiffness.
Apart from permitting a surgeon to check inside a joint for the probable cause of the problem, an arthroscopy is also used to treat a range of conditions that are the reason for pain. These conditions/problems are:
- To repair any damaged cartilage, present in the joints
- To remove fragmented bones or cartilage debris
- To treat shoulder contracture, also known as frozen shoulder or adhesive capsulitis – a condition where there is pain and stiffness in the shoulder joint.
Arthroscopy is also used to examine joints that are very painful due to a bad injury. The examination is done while the patient is under anaesthesia, and it allows the surgeon to thoroughly examine the joint for obvious and subtle issues like joint movement and ligament tears.
Post-surgery, the patient is stabilized in the recovery ward before being taken to their room and generally discharged that day. A bandage will be applied at the site of the surgery, and this can be removed the following day. The punctured wounds will be stitched with paper strips of a single stitch, which will be removed ten days after the procedure. Two weeks after the surgery, using either still pictures or an operative video taken during the surgery, the surgeon will discuss the intra-operative findings after the patient’s joint has been examined.
For those patients who have undergone a knee joint arthroscopy procedure, crutches are generally not advised as they will be able to walk unaided. Within one to two weeks after the surgery, a patient may be able to do light physical activity and resume full physical activity like lifting or sports activity, after six to eight weeks.
There are advantages to having an arthroscopic procedure done:
- Only small incisions are made in the skin and therefore, there will not be large scars marring your skin
- It is less painful than if you had undergone a traditional surgery
- The healing time is much quicker in comparison to traditional surgery
- There is a far lower risk of the wound getting infected
- Finally, the most important of all reasons to have an arthroscopy is that the patient can return to their normal activities very quickly.
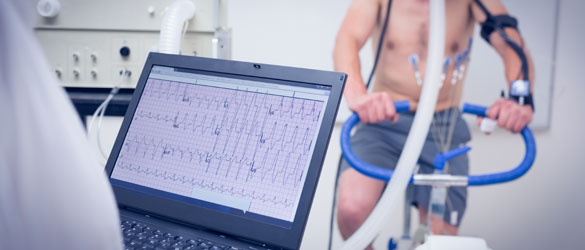
Sports Medicine Centre
Sometimes when engaged in sports activities or while exercising, “sports injuries” can happen, or they can even be accidents. Sports injuries may occur during practice or training sessions. They can even happen due to poor training, improper gear, when a person is not in proper form and due to lack of proper warming up / stretching before embarking on a sports activity. Some of the most common sports injuries include:
- Swollen muscles
- Knee injuries
- Sprains and strains
- Pain along the shin bone
- Pulling a hamstring
- Damaging the Achilles Tendon
- Dislocating bones
- Fractures.
Sports injuries are of two types. They are either chronic or acute in nature. Sudden injuries that occur (while participating in a sports activity or when exercising), like fractures to hands, legs, fingers, toes, or a strained back or sprained ankles, are acute injuries. Indications of an acute injury are:
- Swelling
- Extreme arm or leg weakness
- Sudden severe pain
- Being unable to move a joint naturally
- Unable to place weight on the ankle, leg or foot
- Tenderness in the limbs, wrist or fingers
- Visible signs of a bone or joint that is out of place.
Chronic injuries pertain to pain that occurs after you have been strenuously exercising or after a sports activity and continues to be there for a long time. Constant nagging pain when you play, pain when you exercise, a dull ache when you are resting or swelling are all symptoms of a chronic injury.
Sports injuries, like sprains and strains, are generally treated by the RICE method – rest, ice, compression and elevation of the injured limb.
Anti-inflammatory drugs that are non-steroidal in nature will be prescribed, to reduce the swelling and the pain. Immobilization of the injured area is another form of treatment rendered to patients with sports injuries, so as to prevent more damages from occurring. Casts, leg immobilizers, slings and splints are used to immobilize. Surgery is performed when there are torn tendons or ligaments, and broken bones. Rehabilitation plays a key role in the treatment of patients with sports injuries. Finally, resting plays an important part in the healing of a sports injury. Though moving an injured part is good, adequate rest is also necessary and your doctor will guide you to maintain that balance between rehabilitation and rest.
Ligament damage often occurs from a sports injury. Ligaments are sinewy, strong, elastic bands that surround a joint to support and limit the movement of the joint. The ligaments most prone to get damaged in a sports activity are the knee ligaments and the ankle ligaments. The ligaments tear or get stretched due to twisting during sudden motion.
Reconstructive surgery of a ligament tear is performed only when there is a complete tear of the ligament, which consequently causes instability in the knee or ankle joints. During surgery, the torn ligament is replaced with a piece of a healthy tendon from either the knee cap, ankle, or hamstring. The tendon is grafted into place to hold the knee or ankle joint together.
Frozen Shoulder
Stiffness around the shoulder joint, debilitating pain, and limited range of movement in the shoulder are all symptoms of “Frozen Shoulder” or “Adhesive Capsulitis”. The onset of this disorder is very slow, and to regain the use of the shoulder, free of pain, is also a slow process.
Composition of the Shoulder
The shoulder comprises a ball-and-socket joint. Three bones conjoin to form this joint
- The shoulder blade or scapula
- The collarbone or clavicle
- The upper arm or humerus.
The head of the humerus fits into the shallow socket of the shoulder joint, and the connective tissue, also known as the shoulder capsule, envelops the joint. Synovial fluid present in the shoulder capsule lubricates the shoulder capsule and the joint and thereby enables the shoulder to move more easily.
When the connective tissue in the shoulder capsule becomes rigid due to the formation of tight bands of tissue or adhesions, with a simultaneous decrease in the level of synovial fluid, it causes stiffness and limits the range of motion of the shoulder. This condition is referred to as “Frozen Shoulder”.
- First stage or Freezing Stage – it is a slow process, and with time, the pain increases and becomes worse, consequently leading to loss of motion in the shoulder joint. It takes anywhere from 6 weeks to 9 months for the onset of a freezing shoulder
- In stage two (4 months to 6 months), or the Frozen state, the stiffness in the joint continues, however, the pain may subside slightly. During this stage, daily activities involving the movement of the shoulder will be very difficult
- In the Thawing or third stage, the motion in the shoulder begins to improve, but to regain complete or near normal motion in the shoulder, it may be anywhere from 6 months to 3 years
- Affects people in the age group between 40 – 70 years
- People with chronic ailments like diabetes or suffering from stroke, hypothyroidism, hyperthyroidism, Cardiac and Parkinson’s diseases
- Can be caused by surgery, such as a mastectomy, or due to a fracture or any other injury
The doctor will either conduct a physical examination or request for an X-ray or MRI to rule out other causes or injuries. The Orthopaedic Surgeon may also request an ultrasound if suspecting a thickening of the broad ligament (coracohumeral ligament), which helps strengthen the capsule in the shoulder joint. Thickening of the coracohumeral ligament or CHL is another suggestive factor of adhesive capsulitis or frozen shoulder.
Minimum time taken for a frozen shoulder to regain its normal range of motion or near normalcy, could be 3 years, if left untreated.
The aim of treating a frozen shoulder is to curb pain and to improve the range of motion in the shoulder and to strengthen shoulder.
- Prescription of anti-inflammatory, non-steroidal drugs such as analgesics or ibuprofen
- Injecting Cortisone, a steroidal medication, directly into the shoulder joint
- Physiotherapy and heat treatment – In some cases heat treatment may be employed to loosen the shoulder joint, before performing the stretching and range of motion exercises, which are performed under the supervision of a physiotherapist
When a patient diagnosed with frozen shoulder disorder fails to respond to any of the non-surgical treatments listed above, then surgery will be considered as an option.
The aim of performing surgery is to remove stiffness from the joint and to stretch the connective tissues. This is done either by manipulation under anaesthesia (MUA) or through shoulder arthroscopy.
MUA – This procedure is performed by the Orthopaedic Surgeon. Anaesthesia is administered and the Orthopaedic Surgeon will manipulate the shoulder joint to move, causing the capsule and scar tissue to either tear or stretch, consequently releasing the stiffness and increasing the range of motion.
Surgical Capsular Release or Shoulder Arthroscopy – After anaesthesia has been administered, the Orthopaedic Surgeon will make 2 or 3 tiny, keyhole incisions into the afflicted shoulder. An arthroscope (camera measuring 3 and half millimeters) is inserted into one of the incisions. The images from the camera are projected onto a computer screen. Through the other two incisions, microsurgical instruments are inserted to surgically release the frozen shoulder.
Sometimes, the orthopaedic surgeon may use both the manipulation and arthroscopy procedures simultaneously to get the maximum outcomes.
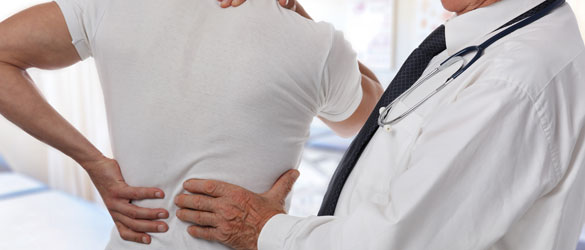
Neck and Lower Back Pain
Posture and lifestyle are key causes for increase in the number of people with back issues. Other causes for backache could include various medical conditions, strenuous work, old age, etc.
This occurs due to a break in one of the vertebrae of the neck (C1-C7). It could happen due to a sudden wrench or impact on the area like a fall, sports injury, whip lash or other contact injuries. There will be pain, swelling, muscle spasms, numbness or tingling at the base of the head. Pain medication, traction, immobilization, halo brace or semi rigid brace may be used as treatment. In severe cases, surgery may be an option.
Neck pain symptoms includes stiffness of the neck, sharp or stabbing pain that radiates down the back or up into the head. Common causes could be sports injuries, poor posture, repetitive motions, whiplash and stress. Depending on the cause, treatment may include rest, heat or cold therapy, medication, physiotherapy and a neck brace.
This usually occurs due to damage to the intervertebral discs, compression of nerve roots, and improper movement of the spinal joints. Rest, pain medication, physiotherapy, cold and hot treatment are the first options. If the back pain is chronic and debilitating, affecting quality of life, surgery may be an option.
Neck sprains occur due to sudden twisting of the neck, bad posture, whiplash, falls etc. Pain medication, physiotherapy, neck exercises, hot and cold therapy, rest and activity modification should ease the neck sprain. A brace may be an option if it is very severe.
Also called compression fractures, they occur more often in women after a certain age. It is due to , when the bone becomes brittle and gets crushed or collapses due to the weight or pull of the surrounding tissues and muscles. It can happen while doing routine activities like turning over in bed, sneezing or coughing. The fracture will be treated first and then the underlying cause, osteoporosis, will be treated. Vertebroplasty and Kyphoplasty are minimally invasive treatments for this kind of fracture.
Clubfoot
Clubfoot is a congenital birth defect, when a child is born with the foot pointed inwards and toes pointing towards each other. In severe cases, the foot may look upside down.
It is usually idiopathic (no particular reason) although it could be due to genetics. It has been linked to skeletal abnormalities in fetus like spina bifida or hip dysplasia. It could be due to disruption in the neuromuscular pathway. Studies have shown that the incidence is more, if the mother is at an advanced age, is a smoker or is diabetic.
The patient will have to wear a brace for a while, after the surgery. Physiotherapy and exercises will be recommended for full recovery. It is better to do the surgery as soon as possible as a child responds better and faster to a surgery than an adult. In many cases, for an adult, several surgeries may be required.
Sometimes, limited surgery may be enough to manipulate the foot into proper alignment. The surgeon will lengthen the Achilles tendon near the heel. The joint capsule in the back of the ankle may need to be released (limited posterior release). The tendon that helps to move the foot may need to be repositioned (tibialis anterior tendon transfer).The ligaments and tendons will be loosened.
If the affliction is severe, the surgeon may need to perform an Osteotomy (cut into the bone to turn the foot). This requires insertion of metal plates or screws to hold the foot in place. Your leg will then be put in a cast. Although there is a recovery time involved, the child is certain to go back to normal life.