Journal Scan
A review of 10 recent papers of immediate clinical significance, harvested from major international journals
From the desk of the Editor-in-Chief
(1). Rebecca Morelle. Scans reveal how Covid may change the brain. 2022.
https://www.bbc.com/news/health-60591487
Catching Covid may cause changes to the brain, a study suggests.
Scientists found significant differences in MRI (magnetic resonance imaging) scans before and after infection.
Even after a mild infection, the overall size of the brain had shrunk slightly, with less grey matter in the parts related to smell and memory.
The researchers do not know whether the changes are permanent but stressed the brain could heal.
The study is published in the journal Nature.
Lead author Prof Gwenaelle Douaud, from the Wellcome Centre for Integrative Neuroimaging, at the University of Oxford, said: “We were looking at essentially mild infection, so to see that we could really see some differences in their brain and how much their brain had changed compared with those who had not been infected was quite a surprise.”
The UK Biobank project has followed the health of 500,000 people for about 15 years and has a database of scans recorded before the pandemic so provided a unique opportunity to study the long-term health impacts of the virus.
The scientists rescanned: 401 participants 4.5 months, on average, after their infection, 96% of whom had had mild Covid, and 384 participants who had not had Covid
They found:
- The overall brain size in infected participants had shrunk between 0.2 and 2%
- There were losses in grey matter in the olfactory areas, linked to smell, and regions linked to memory
- Those who had recently recovered from Covid found it a bit harder to perform complex mental tasks
But the researchers do not know whether the changes are reversible or truly matter for health and wellbeing.
“We need to bear in mind that the brain is really plastic – by that we mean it can heal itself – so there is a really good chance that, over time, the harmful effects of infection will ease,” Prof Douaud said.
The most significant loss of grey matter was in the olfactory areas – but it is unclear whether the virus directly attacks this region or cells simply die off through lack of use after people with Covid lose their sense of smell.
It is also unclear whether all variants of the virus cause this damage.
The scans were performed when the original virus and alpha variant were prevalent and loss of smell and taste a primary symptom.
But the number of people infected with the more recent Omicron variant reporting this symptom has fallen dramatically.
Paula Totaro lost her sense of smell when she caught Covid, in March 2020. “When it was gone, it was like living in a bubble or a vacuum – I found it really isolating,” she said.
But after contacting AbScent, which supports people who have lost their ability to smell and taste, she began smell training.
“What smell training does – particularly if you do it twice a day, regularly, religiously – is it forces you to take the smell, allow it to go back into your nose and then to think about what it is that you’re smelling,” she said.
“And that connection between what’s in the external world and what goes into your brain and your mind is what is being exercised.”
Ms Totaro has now recovered most of her sense of smell – although she still has trouble identifying what different smells are.
“It’s a mix of joy that the sense has come back but still a little bit of anxiety that I’m not quite there yet,” she said.
UK Biobank chief scientist Prof Naomi Allen said: “It opens up all sorts of questions that other researchers can follow up about the effect of coronavirus infection on cognitive function, on brain fog and on other areas of the brain – and to really focus research on how best to mitigate that.”
Prof David Werring, from the University College London Institute of Neurology, said other health-related behaviour could have contributed to the changes seen.”The changes in cognitive function were also subtle and of unclear relevance to day-to-day function,” he said.”And these changes are not necessarily seen in every infected individual and may not be relevant for more recent strains.”
(2). Michelle Roberts. ‘World-first’ heart-thymus transplant success for Easton. 2022.
https://www.bbc.com/news/health-60648869
US doctors say a young boy called Easton has made medical history by becoming the first person in the world to receive a combined heart and thymus transplant.
The pioneering procedure was done to save his life, but could also revolutionise the field of organ transplantation, they hope.
The donated thymus tissue should help stop his body rejecting the new heart.
Months on from the surgery, tests reveal Easton is progressing well.
The thymus tissue is working, meaning his body is building critical immune cells which might ultimately reduce or even eliminate the need for him to take lifelong anti-rejection drugs.
One of his doctors, Joseph Turek from Duke University Hospital, said: “We are very excited about it. This concept of tolerance has always been the holy grail in transplantation, and we are now on the doorstep.
“This has the potential to change the face of solid organ transplantation in the future.”
The thymus gland helps the development of T-cells, which fight foreign substances in the body. It teaches these immune cells what is “self” and what isn’t, and therefore what can be attacked.
Giving Easton cultured thymus tissue from the same donor who gave him a heart, should help his body adopt the new tissues, his doctors believe.
Easton’s story:
Easton was born with a weak heart as well as problems with his immune system. He spent his first seven months in hospital – some of it on life support – and needed numerous heart operations. as well as treatment for recurrent infections that his body was unable to fight on its own.
His mother, Kaitlyn Sinnamon, recalls: “It helped some, but it was basically a band aid for us to make it through transplant.”
His doctors applied to the medical regulatory body, the FDA, to carry out an experimental type of transplant that hadn’t been done in combination before, as far as they knew.
Since Easton needed a new heart and, independently, a new thymus gland, the FDA granted approval for the procedures that went ahead in August 2021, when Easton was six months old.
Dr Turek said: “This was very serendipitous. We had the expertise to do both.
“The work we had done in the laboratory was based around using thymus along with heart transplantation in order to develop tolerance – so basically retraining the immune system and having the thymus of the same donor and heart grow up together.
“We thought this was an opportunity for Easton. This could be applied to all solid organs down the road potentially if this works.”
Much more research is needed before then, including checking if it is viable to remove and replace the thymus in people who have one that is already fully functioning.
The medical team plan to wean Easton off the immunosuppressive drugs at some point, to see how he progresses.
Kaitlyn said: “I hope that as he gets older he gets to be proud of his scars, and know that he not only got to save his own life, but got to save other people’s lives as well.”
(3). Chris Harding, et al. Alternative to prophylactic antibiotics for the treatment of recurrent urinary tract infections in women: multicentre, open label, randomised, non-inferiority trial. BMJ 2022;376:e068229
Abstract
Objective: To test and compare the efficacy of methenamine hippurate for prevention of recurrent urinary tract infections with the current standard prophylaxis of daily low dose antibiotics.
Design: Multicentre, open label, randomised, non-inferiority trial.
Setting: Eight centres in the UK, recruiting from June 2016 to June 2018.
Participants: Women aged ≥18 years with recurrent urinary tract infections, requiring prophylactic treatment.
Interventions: Random assignment (1:1, using permuted blocks of variable length via a web-based system) to receive antibiotic prophylaxis or methenamine hippurate for 12 months. Treatment allocation was not masked and crossover between arms was allowed.
Main outcome measure: Absolute difference in incidence of symptomatic, antibiotic treated, urinary tract infections during treatment. A patient and public involvement group predefined the non-inferiority margin as one episode of urinary tract infection per person year. Analyses performed in a modified intention-to-treat population comprised all participants observed for at least six months.
Results: Participants were randomly assigned to antibiotic prophylaxis (n=120) or methenamine hippurate (n=120). The modified intention-to-treat analysis comprised 205 (85%) participants (antibiotics, n=102 (85%); methenamine hippurate, n=103 (86%)). Incidence of antibiotic treated urinary tract infections during the 12-month treatment period was 0.89 episodes per person year (95% confidence interval 0.65 to 1.12) in the antibiotics group and 1.38 (1.05 to 1.72) in the methenamine hippurate group, with an absolute difference of 0.49 (90% confidence interval 0.15 to 0.84) confirming non-inferiority. Adverse reactions were reported by 34/142 (24%) in the antibiotic group and 35/127 (28%) in the methenamine group and most reactions were mild.
Conclusion: Non-antibiotic prophylactic treatment with methenamine hippurate might be appropriate for women with a history of recurrent episodes of urinary tract infections, informed by patient preferences and antibiotic stewardship initiatives, given the demonstration of non-inferiority to daily antibiotic prophylaxis seen in this trial.
(4). Paul Farmer, Obituary. Lancet. 2022;399.
Global health pioneer. Born on Oct 26, 1959 in North Adams, MA, USA, he died after an acute cardiac event on Feb 21, 2022 in Butaro, Rwanda, aged 62 years.
A global health visionary who commanded the attention of world leaders, Paul Farmer “considered himself a physician to the poor first”, said Joia Mukherjee, Chief Medical Officer of Partners In Health (PIH). Farmer was tireless in his efforts to improve health services for marginalised communities and to demand correctives to the underlying structures that perpetuated global inequities. He was “absolutely unwilling to accept that we couldn’t provide modern, high quality medical care to the poor. I believe he will go down in history as a really great moral philosopher in always having one standard of care and justice”, Mukherjee said. “I will always be in awe of his vision and his passion to fulfil that vision”, said Anthony Fauci, Director of the US National Institute of Allergy and Infectious Diseases. “He will long be remembered as a once-in-a-lifetime icon public health hero, who brought true meaning to the concept of health equity.”
After graduating from Duke University, Durham, NC, USA, with a bachelor’s degree in medical anthropology in 1982, Farmer went to volunteer in Haiti. His experiences there jump-started a “lifelong fascination with rights, not just to the right to vote or other civil and political rights, but also the right to eat and the right to have access to health care”, he later recalled. With Ophelia Dahl, he founded a small comm unity clinic there in 1983. Even as he jointly pursued a medical degree from Harvard Medical School (HMS) and a doctorate in medical anthropology from Harvard University, USA, he returned to the clinic regularly, covertly ferrying suppliesfrom Boston. With Dahl and three other co-founders, Farmer created PIH in 1987, a non-profit based in Boston to supportthe work in Haiti. PIH now works across four continents assisting governments to deliver sustainable health care tomarginalised communities. As PIH’s Chief Strategist, Farmer guided its development. “His intellectual scholarship served to tie health to political economy and history. He laid the scholarly foundation for why we must preferentially treat the destitute sick, and did the work to show the world how to it”, Mukherjee said. He challenged assumptions about what could be achieved in remote, poor settings, including leading efforts to deliver the highest standard of HIV treatment to patients in rural Haiti beginning in 1998, when policy makers argued that it was not possible or cost-effective. He also made advances in the treatment of drug-resistant tuberculosis. “He believed morally that everyone deserved treatment”, said Arthur Kleinman, a Professor of Medical Anthropology, Global Health, and Psychiatry at Harvard.
As a practitioner of social medicine, Farmer highlighted the world’s “medical deserts”, drawing connections between inadequate health services in those places and the impacts of colonialism and other extractive policies. He demanded reparations for those communities and the protection of their human rights. “He saw the foundation of global health, not just as infectious diseases and biomedicine and established public health practices, but to see those things brought together with social theory, ethnography, and history. That was Paul’s brilliance,” Kleinman said. Recently, Farmer had joined calls to address disparities in global access to COVID-19 vaccines and treatments with a waiver on patent protections.
While his work with PIH served as the practical application of his philosophy, he valued his roles as a writer, speaker, and educator. In 2009, he became Chair of HMS’s Department of Global Health and Social Medicine and was named the Kolokotrones University Professor the next year. “Paul was inspirational to everybody around him. He really showed us how to be caring clinicians”, said Eugene Richardson, Assistant Professor of Global Health and Social Medicine at HMS. Farmer also headed the Division of Global Healthy Equity at Brigham and Women’s Hospital in Boston, which, along with Harvard anchored his work. “He believed it was the work of teaching hospitals and the work of universities to change the lives of the poorest people”, said Louise Ivers, Professor of Global Health and Social Medicine at HMS. Farmer endeavoured to build new institutions to train nurses and physicians in the communities where he worked, even as he committed to “engage them in his career as collaborators and help them in their own advancement”, Kleinman said. PIH created the University Hospital of Mirebalais in central Haiti after the country’s 2010 earthquake and helped found the University of Global Health Equity (UGHE) in Butaro, Rwanda, in 2015.
Farmer was teaching at UGHE when he died. “He put the poor, the marginal, the disabled…he put them first”, Kleinman said. Farmer is survived by his wife, Didi Bertrand Farmer, and their three children, Catherine, Elizabeth, and Sebastian. Paul Farmer: public health and social medicine visionary
Paul Farmer’s humanitarian passion was summed up in the title of the book by Pulitzer Prize winning author Tracy Kidder: Mountains Beyond Mountains: The Quest of Paul Farmer, A Man Who Would Cure the World.
Farmer, a “social medicine” practitioner, Harvard medical school professor, anthropologist, and author of 12 books, delivered high quality healthcare to some of the world’s poorest people. His mantra was that the biggest failure in bringing healthcare to them was one of imagination.
He said, “Many use the metaphor of a clinical desert, a place where you don’t have the tools of the trade. Can that be irrigated? Of course it can. If you can build a hospital adjacent to a battlefield, then you can certainly do it after the battle is over – like in Sierra Leone, Liberia, Peru, or Guatemala after civil war, in Haiti when the coups stop, in Rwanda after the genocide against the Tutsi.”
Healthcare, he insisted, was not an island. Patients needed access to food, transport, and housing. A mother could not have cancer care and lose work without economic support; a patient with tuberculosis could not endure strong drugs on an empty stomach; illness had social roots and had to be tackled through social structures.
Student idealism fired his pursuit of “global health equity” and dream to build a clinic in Cange, Haiti, where he lived in a squatter settlement with people who struggled to feed their families
(5). Maura Marcucci, et al. Benefits and harms of direct oral anticoagulation and low molecular weight heparin for thromboprophylaxis in patients undergoing non-cardiac surgery: systematic review and network meta-analysis of randomised trials. BMJ 2022;376:e066785.
Abstract
Objective: To systematically compare the effect of direct oral anticoagulants and low molecular weight heparin for thromboprophylaxis on the benefits and harms to patients undergoing non-cardiac surgery.
Design: Systematic review and network meta-analysis of randomised controlled trials.
Data sources: Medline, Embase, and the Cochrane Central Register of Controlled Trials (CENTRAL), up to August 2021.
Review methods: Randomised controlled trials in adults undergoing non-cardiac surgery were selected, comparing low molecular weight heparin (prophylactic (low) or higher dose) with direct oral anticoagulants or with no active treatment. Main outcomes were symptomatic venous thromboembolism, symptomatic pulmonary embolism, and major bleeding. Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines were used for network meta-analyses. Abstracts and full texts were screened independently in duplicate. Data were abstracted on study participants, interventions, and outcomes, and risk of bias was assessed independently in duplicate. Frequentist network meta-analysis with multivariate random effects models provided odds ratios with 95% confidence intervals, and GRADE (grading of recommendations, assessment, development, and evaluation) assessments indicated the certainty of the evidence.
Results: 68 randomised controlled trials were included (51 orthopaedic, 10 general, four gynaecological, two thoracic, and one urological surgery), involving 45 445 patients. Low dose (odds ratio 0.33, 95% confidence interval 0.16 to 0.67) and high dose (0.19, 0.07 to 0.54) low molecular weight heparin, and direct oral anticoagulants (0.17, 0.07 to 0.41) reduced symptomatic venous thromboembolism compared with no active treatment, with absolute risk differences of 1-100 per 1000 patients, depending on baseline risks (certainty of evidence, moderate to high). None of the active agents reduced symptomatic pulmonary embolism (certainty of evidence, low to moderate). Direct oral anticoagulants and low molecular weight heparin were associated with a 2-3-fold increase in the odds of major bleeding compared with no active treatment (certainty of evidence, moderate to high), with absolute risk differences as high as 50 per 1000 in patients at high risk. Compared with low dose low molecular weight heparin, high dose low molecular weight heparin did not reduce symptomatic venous thromboembolism (0.57, 0.26 to 1.27) but increased major bleeding (1.87, 1.06 to 3.31); direct oral anticoagulants reduced symptomatic venous thromboembolism (0.53, 0.32 to 0.89) and did not increase major bleeding (1.23, 0.89 to 1.69).
Conclusions: Direct oral anticoagulants and low molecular weight heparin reduced venous thromboembolism compared with no active treatment but probably increased major bleeding to a similar extent. Direct oral anticoagulants probably prevent symptomatic venous thromboembolism to a greater extent than prophylactic low molecular weight heparin.
(6). Victoria E Kettle, et al. Effectiveness of physical activity interventions delivered or prompted by health professionals in primary care settings. BMJ 2022;376:e068465.
Abstract
Objective: To examine the effectiveness of physical activity interventions delivered or prompted by primary care health professionals for increasing moderate to vigorous intensity physical activity (MVPA) in adult patients.
Design: Systematic review and meta-analysis of randomised controlled trials.
Data sources Databases (Medline and Medline in progress, Embase, PsycINFO, CINAHL, SPORTDiscus, Sports Medicine and Education Index, ASSIA, PEDro, Bibliomap, Science Citation Index, Conference Proceedings Citation Index), trial registries (Cochrane Central Register of Controlled Trials, ClinicalTrials.gov, TRoPHI), and grey literature (OpenGrey) sources were searched (from inception to September 2020).
Eligibility criteria for selecting studies Randomised controlled trials of aerobic based physical activity interventions delivered or prompted by health professionals in primary care with a usual care control group or another control group that did not involve physical activity.
Study selection and analysis:Two independent reviewers screened the search results, extracted data from eligible trials and assessed the risk of bias using the Cochrane risk of bias tool (version 2). Inverse variance meta-analyses using random effects models examined the primary outcome of difference between the groups in MVPA (min/week) from baseline to final follow-up. The odds of meeting the guidelines for MVPA at follow-up were also analysed.
Results: 14 566 unique reports were identified and 46 randomised controlled trials with a range of follow-ups (3-60 months) were included in the meta-analysis (n=16 198 participants). Physical activity interventions delivered or prompted by health professionals in primary care increased MVPA by 14 min/week (95% confidence interval 4.2 to 24.6, P=0.006). Heterogeneity was substantial (I2=91%, P<0.001). Limiting analyses to trials that used a device to measure physical activity showed no significant group difference in MVPA (mean difference 4.1 min/week, 95% confidence interval −1.7 to 9.9, P=0.17; I2=56%, P=0.008). Trials that used self-report measures showed that intervention participants achieved 24 min/week more MVPA than controls (95% confidence interval 6.3 to 41.8, P=0.008; I2=72%, P<0.001). Additionally, interventions increased the odds of patients meeting guidelines for MVPA by 33% (95% confidence interval 1.17 to 1.50, P<0.001; I2=25%, P=0.11) versus controls. 14 of 46 studies were at high risk of bias but sensitivity analyses excluding these studies did not alter the results.
Conclusions: Physical activity interventions delivered or prompted by health professionals in primary care appear effective at increasing participation in self-reported MVPA. Such interventions should be considered for routine implementation to increase levels of physical activity and improve health outcomes in the population.
(7). Ian R Reid, et al. Drug therapy for osteoporosis in older adults. Lancet 2022;399(10329):P1080-92.
Summary
The goal of osteoporosis management is to prevent fractures. Several pharmacological agents are available to lower fracture risk, either by reducing bone resorption or by stimulating bone formation. Bisphosphonates are the most widely used anti-resorptives, reducing bone turnover markers to low premenopausal concentrations and reducing fracture rates (vertebral by 50-70%, non-vertebral by 20-30%, and hip by ~40%). Bisphosphonates bind avidly to bone mineral and have an offset of effect measured in months to years. Long term, continuous use of oral bisphosphonates is usually interspersed with drug holidays of 1-2 years, to minimise the risk of atypical femoral fractures. Denosumab is a monoclonal antibody against RANKL that potently inhibits osteoclast development and activity. Denosumab is administered by subcutaneous injection every 6 months. Anti-fracture effects of denosumab are similar to those of the bisphosphonates, but there is a pronounced loss of anti-resorptive effect from 7 months after the last injection, which can result in clusters of rebound vertebral fractures. Two classes of anabolic drugs are now available to stimulate bone formation. Teriparatide and abaloparatide both target the parathyroid hormone-1 receptor, and are given by daily subcutaneous injection for up to 2 years. Romosozumab is an anti-sclerostin monoclonal antibody that stimulates bone formation and inhibits resorption. Romosozumab is given as monthly subcutaneous injections for 1 year. Head-to-head studies suggest that anabolic agents have greater anti-fracture efficacy and produce larger increases in bone density than anti-resorptive drugs. The effects of anabolic agents are transient, so transition to anti-resorptive drugs is required. The optimal strategy for cycling anabolics, anti-resorptives, and off-treatment periods remains to be determined.
(8). Wouter van der Steen. Safety and efficacy of aspirin, unfractionated heparin, both, or neither during endovascular stroke treatment (MR CLEAN-MED): an open-label, multicentre, randomised controlled trial. Lancet 2022;399(10329);p1023-1092.
Summary
Background
Aspirin and unfractionated heparin are often used during endovascular stroke treatment to improve reperfusion and outcomes. However, the effects and risks of anti-thrombotics for this indication are unknown. We therefore aimed to assess the safety and efficacy of intravenous aspirin, unfractionated heparin, both, or neither started during endovascular treatment in patients with ischaemic stroke.
Methods
We did an open-label, multicentre, randomised controlled trial with a 2 × 3 factorial design in 15 centres in the Netherlands. We enrolled adult patients (ie, ≥18 years) with ischaemic stroke due to an intracranial large-vessel occlusion in the anterior circulation in whom endovascular treatment could be initiated within 6 h of symptom onset. Eligible patients had a score of 2 or more on the National Institutes of Health Stroke Scale, and a CT or MRI ruling out intracranial haemorrhage. Randomisation was done using a web-based procedure with permuted blocks and stratified by centre. Patients were randomly assigned (1:1) to receive either periprocedural intravenous aspirin (300 mg bolus) or no aspirin, and randomly assigned (1:1:1) to receive moderate-dose unfractionated heparin (5000 IU bolus followed by 1250 IU/h for 6 h), low-dose unfractionated heparin (5000 IU bolus followed by 500 IU/h for 6 h), or no unfractionated heparin. The primary outcome was the score on the modified Rankin Scale at 90 days. Symptomatic intracranial haemorrhage was the main safety outcome. Analyses were based on intention to treat, and treatment effects were expressed as odds ratios (ORs) or common ORs, with adjustment for baseline prognostic factors. This trial is registered with the International Standard Randomised Controlled Trial Number, ISRCTN76741621.
Findings
Between Jan 22, 2018, and Jan 27, 2021, we randomly assigned 663 patients; of whom, 628 (95%) provided deferred consent or died before consent could be asked and were included in the modified intention-to-treat population. On Feb 4, 2021, after unblinding and analysis of the data, the trial steering committee permanently stopped patient recruitment and the trial was stopped for safety concerns. The risk of symptomatic intracranial haemorrhage was higher in patients allocated to receive aspirin than in those not receiving aspirin (43 [14%] of 310 vs 23 [7%] of 318; adjusted OR 1.95 [95% CI 1.13-3.35]) as well as in patients allocated to receive unfractionated heparin than in those not receiving unfractionated heparin (44 [13%] of 332 vs 22 [7%] of 296; 1.98 [1.14-3.46]). Both aspirin (adjusted common OR 0.91 [95% CI 0.69-1.21]) and unfractionated heparin (0.81 [0.61-1.08]) led to a non-significant shift towards worse modified Rankin Scale scores.
Interpretation
Periprocedural intravenous aspirin and unfractionated heparin during endovascular stroke treatment are both associated with an increased risk of symptomatic intracranial haemorrhage without evidence for a beneficial effect on functional outcome.
(9). Jakob Lillemoen Drivenes, et al. A girl with unruly locks: molecular genetics makes a diagnosis of uncombable hair syndrome. Lancet 2022;399(10329):P1079.
A 3-year-old girl was referred to the dermatology department with blonde, straw-like, and unruly hair. The child’s parents reported that since birth her hair had been sparse and slow-growing. And from about one year of age, her parents had difficulty combing her hair.
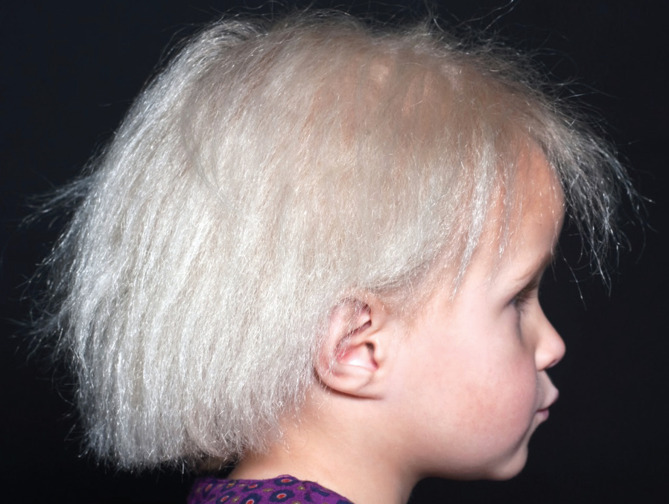
On clinical examination of the patient’s scalp hair, we found the patient had blonde, dry, and glistening hair (figure); her eyebrows and eyelashes were unaffected. Examination of the hair using light microscopy showed irregular triangle-shaped hair shafts and atypical canals along the hair shaft axis.
Molecular genetic analysis showed the homozygous pathogenic variant c.881C>T (p.Ala294Val) in exon 8 of the PADI3 gene.
Considering together the findings from clinical examination, light microscopy, and genetic analysis, we made a diagnosis of uncombable hair syndrome: a rare hair shaft anomaly that presents in early childhood with blond, glistening, and frizzy hair.
Patients’ scalp hair grows in thick bundles that project out in different directions which makes combing impossible. Additionally, in some cases the rate of hair growth may be slow. Under light microscopy, the hair shafts may appear unaffected, and scanning electron microscopy may be necessary to confirm the presence of triangulated hair shafts and longitudinal grooves along the hair shaft axis. No definitive treatment is yet available, but oral biotin supplementation has been reported to make clinical improvement in some cases. The prognosis is promising as hair texture improves during puberty. In some cases, the condition is associated with brachydactyly, ectodermal dysplasia, juvenile cataract, and oligodontia.
Most cases of uncombable hair syndrome-a condition depicted in the 1845 German children’s book Der Struwwelpeter, which translates as “Shock-headed Peterâ€-are sporadic and autosomal recessive; the responsible pathogenic variants are in the PADI3, TCHH, and TGM3 genes, which encode for proteins involved in hair shaft formation. Employment of molecular genetics in diagnosing this syndrome must now be considered the gold standard. Generally, when diagnosing hair and skin disorders, molecular genetics has the advantage of confirming the clinical diagnosis with greater certainty; risks of family members may also be identified. Additionally, molecular genetic analysis usually only requires saliva or an EDTA blood sample, thus avoiding the employment of more invasive investigations.
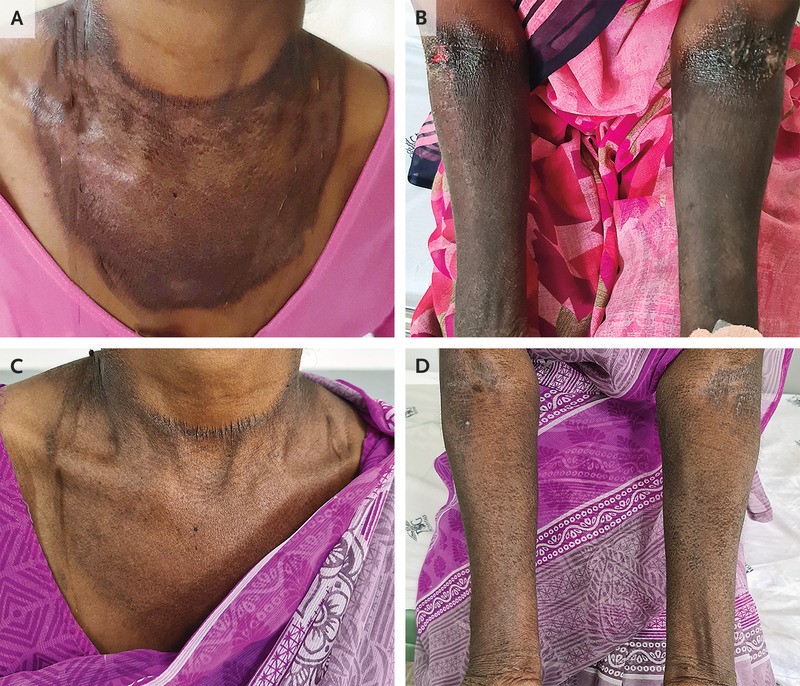
(10). Murali Alagesan, et al. Pellagra. N Engl J Med. 2022;386:e24.
A 48-year-old woman presented to the general medicine clinic with a 6-month history of a worsening rash on her neck and arms. She also reported having diarrhea, fatigue, and loss of appetite, with an 8 kg weight loss over the same period; she had no neurologic symptoms. The patient lived in rural India, adhered to a vegetarian diet, and did not use alcohol. On physical examination, there were well-demarcated areas of hyperpigmentation on the sun-exposed areas of her neck and anterior chest (Panel A) and forearms (Panel B), with skin fissures in the antecubital fossa. Serum niacin testing was unavailable. A diagnosis of pellagra, or niacin deficiency, was made on the basis of the patient’s syndrome of diarrhea and symmetric, photosensitive dermatitis, including a typical Casal’s necklace rash. Pellagra that is caused by dietary deficiency persists in resource-limited countries, whereas it is associated more with alcohol use, bariatric surgery, or malabsorptive conditions in resource-rich countries. After the patient was treated with intravenous vitamin B complex followed by oral supplementation, the diarrhea resolved and the skin hyperpigmentation was reduced at follow-up 4 weeks later.