Most people get to know about jaundice very early in childhood; a bout of viral hepatitis is the common scenario either in oneself (or) in near/known ones. Thus, this form of hepatic origin jaundice gets etched in memory where in bland diet, bed rest & some tonics recover the self-limiting condition (At least in most cases!)
There is another form of jaundice, which does not respond to any of aforementioned treatments and that which requires either intervention (or) surgery to get relief. It is called by terminology of Extrahepatic Cholestatic Jaundice -for simple understanding terms, “The Obstructive Jaundice”.
This type has no major relation to liver disease and results from blockage of bile passage. Bile (or) Pith is responsible for fat digestion in intestines. Thus, any condition, which obstructs the passage of bile from its origin in the liver to its destination, the upper small intestine results in “Obstructive Jaundice.” (Ref: Fig 1)
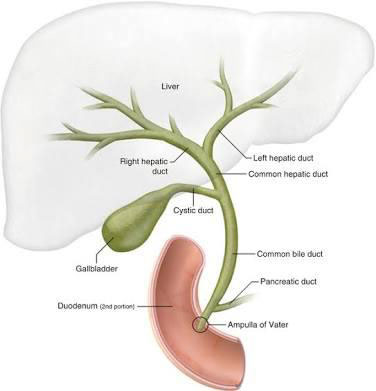
This Schematic diagram represents bile passage from its origin in liver to its destination in upper small intestine where it aids digestion.
Any condition that obstructs this bile flow causes “Obstructive Jaundice”
The obstructing factor may be a stone or stricture or cancer in most cases. Differentiating the very many causes requires thorough clinical assessment / appropriate laboratory tests, imaging (CT vs MRCP). Once the cause is ascertained, it becomes easier to plan a strategy to relieve the obstruction. The treatment options available include
(1) ERCP -(ENDOSCOPIC INTERVENTION)
- Very commonly used/appropriate in most indications
- Done by gastroenterology experts via endoscope
- avoids surgery
(2) PTBD-(RADIOLOGICAL INTERVENTION)
- Alternative to ERCP
- Useful if obstruction is close to liver
- Done by radiologists
- Useful in select indications
(3) SURGERY
- Last resort
- Definitive in select cases
- may even be done on “palliative” basis in few cases
The type of treatment is usually decided on case to case basis depending on level of obstruction, type of obstruction, comorbid conditions and technical feasibility.
Thus jaundice is not always what one tends to know as common man and requires urgent consultation with specialists in the field, as sometimes this decision may even be lifesaving in the background of biliary infection caused by obstructive jaundice.

Dr. M. A. Arvind, MBBS, MD (General Medicine), DM(Gastro)
Consultant Medical Gastroenterologist
Kauvery Hospital, Chennai

