We dermatologists in our day to day practice are confronted with a common question from patients.
Doctor, I hope I am not suffering from Psoriasis. He or she would have come with a completely unrelated condition; mostly mild but sometimes bizarre scenarios are encountered where patients with much more serious skin conditions like Pemphigus keep pestering us wanting us to rule out Psoriasis.
So why is there so much fuss & anxiety about this condition not seen with any other skin condition?
A possible reason could be the splashing of photographs of patients suffering from relatively rare severe forms of the disease in the media advertisements (both print & visual) of some non-allopathic centre claiming to treat psoriasis. Another reason could be incorrect & misleading information from various internet sites &social media platforms.
The aim of this write-up is to present a few basic facts before the public to help them understand this condition in a meaningful way so that the fear & stigma associated with this condition can be allayed at least to a certain extent.
Also Read: Functions of Skin and Skin Care
Psoriasis
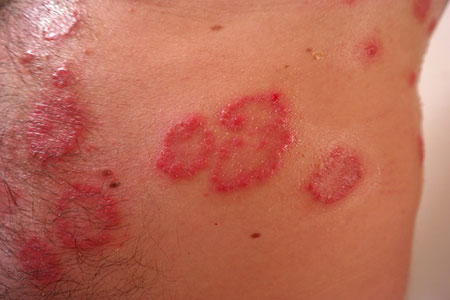
Psoriasis is a chronic inflammatory skin disorder characterized by well demarcated red elevated areas of skin with silvery scales commonly affecting extensor surfaces of the body like elbows; knees etc. Scalp involvement is seen frequently. Palms & soles can also be involved. Guttate & napkin psoriasis are some variants seen in children. Erythrodermic & pustular forms constitute the uncommon severe forms of the disease. Certain nail changes are characteristic of Psoriasis. In addition to skin, Psoriasis can also involve joints in a subset of patients (Psoriatic arthritis).
Men and women are equally affected. It can also occur in childhood
Psoriasis is not an infectious or contagious disease.
There is no clear link between diet & severity of psoriasis.
Psoriasis is referred to as mild to moderate when less than 10% body surface area is involved & severe when greater than 10% body surface area is involved.
About 30% of patients have a positive family history. The pattern of inheritance is multifactorial with multiple susceptibility loci.
Factors triggering or exacerbating psoriasis include infections, stress, trauma, certain medications (Lithium, Beta-blockers, and Anti-malarials etc.), smoking & alcohol consumption.
Psoriasis can be associated with metabolic syndrome (abdominal obesity, hypertension, insulin resistance, dyslipidemia). Studies have suggested that people with psoriasis may have an increased risk of cardiovascular disease. Therefore psoriatic patients need to be monitored regularly to identify & treat the risk factors which may lead to cardiovascular disease.
Psoriasis is managed in an outpatient setting most of the time.
Pustular & erythrodermic psoriasis may need a short spell of hospital admission to stabilize metabolic parameters which could be deranged in these conditions.
Management of Psoriasis involves topical therapy, phototherapy, systemic & biologic therapies.
Topical therapy alone is helpful when the area of involvement is less than 10% body surface area.
Topical therapies in Psoriasis include topical steroids, coal tar preparations, retinoids like tazarotene and Vitamin D3 analogues like Calcipotriol.
When there is more than 10% body surface area involvement systemic therapies are added to topical therapies. Systemic options in Psoriasis include Methotrexate, Acitretin, and Cyclosporine.
Phototherapy especially Narrow band UVB phototherapy is another useful option in the management of extensive psoriasis in a few patients.
The treating dermatologist tailors the medications individually according to the need of each patient. When there is arthropathy, a rheumatologist is also involved in patient care to optimize & improve treatment outcomes.
In recent years, a new modality of systemic therapy-biologic therapy (etanercept, infliximab, secukinumab etc.) is revolutionizing Psoriasis management, leading to the faster clearing of lesions & greater reduction of areas of involvement and improvement of joint symptoms.
Psoriasis is a chronic disease like diabetes. It can be managed well & maintained under good control in a vast majority of patients. Patients can carry on with their lives with minimal inconveniences as with any chronic illness. There can be a few flares & setbacks along the way, but they can be taken care of by the treating dermatologist and/or rheumatologist. Adherence to advised treatment is very important as the abrupt stopping of prescribed medication by the patient can lead to exacerbation of skin & joint symptoms.
There is no cure for psoriasis at this point of time. Research on psoriasis is going on all over the world & in the last decade, great strides have been made in understanding what goes wrong in psoriasis & so there is good cause for optimism.
![Best Dermatologist in Chennai, India | Psoriasis treatment| Kauvery Hospital Dr. Vijay Kartik -Dec-11-2015-04-01-41-Dr_V_VIJAY_KARTIK[1]](https://www.kauveryhospital.com/images/newsletters/2017_inside/Dr.%20Vijay%20Kartik%20-Dec-11-2015-04-01-41-Dr_V_VIJAY_KARTIK%5B1%5D.jpg)
Article by Dr. Vijay Kartik, MBBS., DVD,
Consultant Dermatologist,
Kauvery Hospital, Chennai