Amongst all the chaos of the COVID 19 pandemic across the world and in our city, as Emergency physicians we find there is a tendency of people to avoid visiting the hospital for various reasons. The top 3 reasons being:
- Fear of contracting Covid 19 infection while visiting the hospital
- If suspected of Covid infection – the fear of social isolation and quarantine
- Lockdown across the city, making it difficult to commute for medical aid while many hospitals are also under lockdown for services to patients.
Over the last 1 month, as an Emergency physician working in the Emergency Department, we have seen a number of patients who have come with delayed presentations for acute emergencies and have landed up in several complications.
-
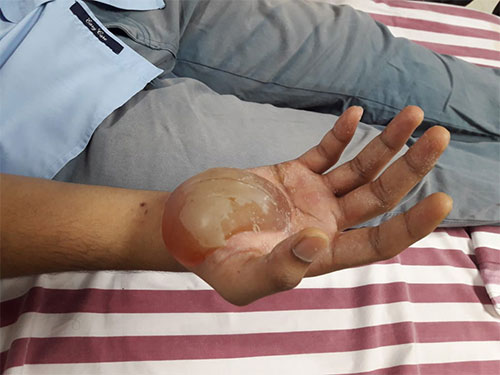
- We had a patient – young gentleman in his early 30s, and he came to us with a history of accidental burns to his right palm while cooking at home when he accidentally touched the hot vessel. The incident happened about a week before he visited our Emergency Department.
On examination: he was found to have a huge blister extending almost all over the right palm with fluid within the blister along with the spread of that infection over the hand and wrist. He was diagnosed to have a 2nd degree deep burn – 2% of total body surface area with superadded early signs of cellulitis of hand and forearm.
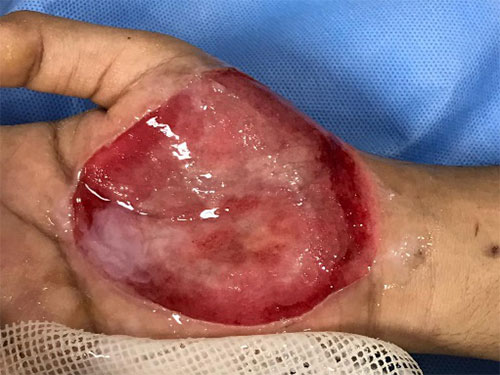
2nd degree deep burns over right palm After incision drainage & deroofing the blister - This was treated with immediate Incision and drainage of the fluid and deroofing of the blister and a burns dressing keeping the Plastic Surgeon Team in the loop. The patient was also treated with IV antibiotics and analgesics.
- This was a complication that could be easily avoided without superadded infection, had it been attended to in the first 24 to 48 hrs.
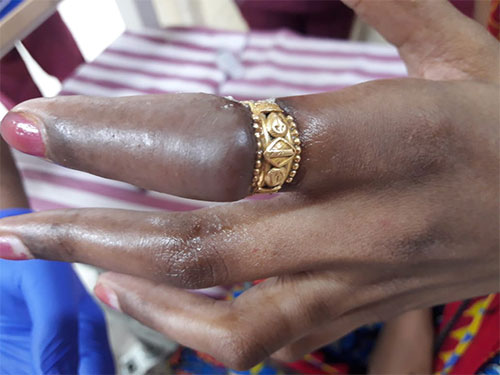
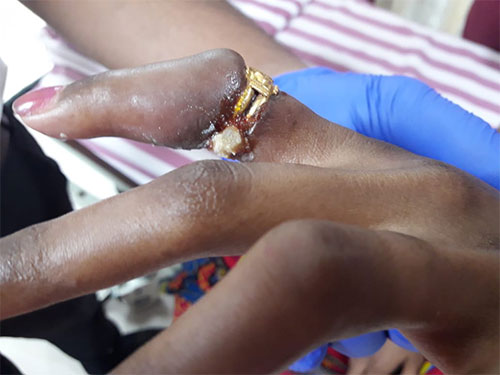
- A young lady around 24 years of age, was brought to us with h/o ring getting stuck in her finger on day 4, initially she was treated at a local clinic where they mentioned non-availability of specialist doctors to treat her condition, thereby she tried to remove the ring on her own which led to skin ulceration, induration and impending vascular compromise to that finger. She came to us with a lot of pain and skin colour change over her distal part of the finger.
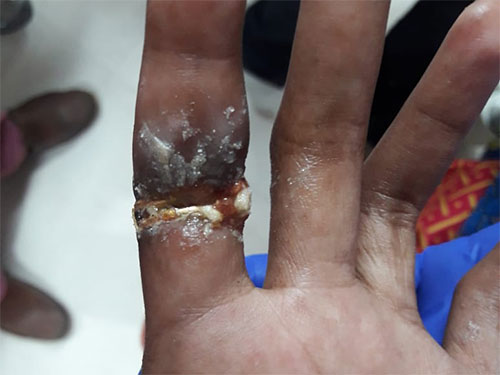
Ring constriction causing bluish discolouration over distal aspect of finger Ring causing ulceration & infection due to induration Ring constriction leading to vascular compromise & superadded infection - This was again treated under a Digital Block (local anaesthetic block) and removal of the ring was done by the emergency Physician and subsequent restoration of the vascular supply to the finger and she was referred to the Plastic Surgery team for follow up and management.
- In such cases, vascular compromise of the finger can lead to severe complications that could have led to the loss of the entire finger had the patient presented to us with a bit more delay. These are emergencies that need to be addressed as soon as possible as timely intervention can be limb saving.
- Another such presentation of a 60-year lady, known to have Hypertensive and Diabetic, presented to us after 1 week history of abdominal pain and constipation for 3 days along with h/o inability to pass flatus for 3 days and persistent multiple episodes of vomiting for 3 days – treated with self-medication with multiple oral antibiotics, antacid and antiemetics. On presentation to us, she seemed to have an obstructed incisional hernia which was irreducible and on evaluating her after basic labs and CT scan of the abdomen – she was found to have a small intestine obstruction with acute kidney injury secondary to infection and dehydration. She was immediately taken up for emergency surgery by the Surgical Gastroenterologist for hernia mesh repair and treated with IV fluids, IV antibiotics, strict sugar control (as per advice of the Diabetologist) and measures to ensure kidney function is corrected back to normal (as per advice of the nephrologist) and then discharged home after 5 days once her kidney functions were back to normal.
One must remember:– Had the patient presented to us a lot later – there could be complications like bowel ischemia, bowel gangrene (complete cut off of blood supply to the intestine) or even perforation and peritonitis (where the intestine bursts and fecal contents contaminate the abdomen) with the possibility of worsening multiple organ dysfunction – which could have been life threatening.
– Again, delay in the presentation was due to fear of hospitalization and fear of contracting covid during hospital stay.
- A young pregnant lady in her first trimester around 9 weeks of pregnancy presented to us with h/o severe abdominal pain over the right lower abdomen since more than 10 hrs. She had a UPT card test done at home which was found to be positive about 3 weeks ago. But due to lockdown she was not able to go for a regular obstetric check-up. She presented to us late at night with worsening symptoms of pain. On examination, she had severe right lower abdomen tenderness and an emergency ultrasound scan was done by our on-call radiologist which showed her to have a right fallopian tubal pregnancy impending rupture. She was immediately taken up for emergency surgery by the on-call Gynecologist and was found to have tubal pregnancy where the fetal sac was ruptured within the fallopian tube causing bleeding slowly within the tube.- Had this patient presented to us much later – there would have been high chances of tubal rupture and hemorrhage leading to death if not treated on time.
- We had a patient – young gentleman in his early 30s, and he came to us with a history of accidental burns to his right palm while cooking at home when he accidentally touched the hot vessel. The incident happened about a week before he visited our Emergency Department.
The list of medical and surgical emergencies is endless, and these could be time-critical emergencies if not treated on time can be life-threatening: To name a few that need immediate attention:
-
-
- Acute heart attacks are best treated with good reversibility of cardiac function if treated on time and the golden hour is 1 hour from the onset of pain. Delay in treatment can cause complications like irreversible muscle damage leading to pumping failure, fatal abnormalities in the electrical conduction of the heart leading to very low or very high pulse rate which can lead to sudden death if not treated on time.
- Acute onset strokes are best treated within 4.5 to 6 hours of the onset of symptoms. Still, delay in presentation to hospital beyond this golden hour can lead to severe morbidity, disability and mortality.
- Patients with trauma at home secondary to accidental falls or RTAs – whether limb fracture or head injuries, they should be addressed on time to prevent complications.
- Any patients on Dialysis need timely interventions to ensure life-threatening complications are avoided.
-
Here, at Kauvery Hospital – our department of emergency medicine, is open round the clock for all medical and surgical emergencies with a well-experienced team of emergency physicians, emergency nursing staff and emergency technicians who strive to ensure the patient gets the best quality of care and expert speciality advice.
To ensure the safe travel of the patient from their location to the hospital we have 24×7 ambulance service with a well-trained emergency paramedical technician who start the treatment for patients from the time the patient has been picked up and ensure continuous monitoring of patient’s condition enroute to the hospital.
In the hospital set up too, we have a stringent screening protocol for all patients during this pandemic and fever patients are treated separately in fever clinic and triage room to ensure safety of all patients and to prevent cross-contamination to other patients.
We, are about 12 doctors, 14 nursing staff, 10 paramedical technician staff, 3 coordinators along with other support staff (Housekeeping & Security staff) – are very committed to delivery timely care and ensure the quality of care to all patients, while ensuring all safety precautions during this pandemic.



“Lockdowns are temporary. Care is permanent”, and “our team of medical professionals is ever-ready to care for any medical or surgical emergency round-the-clock”

Dr. Aslesha Vijaay Sheth
Consultant Clinical Lead & Incharge
Department of Emergency Medicine
Kauvery Hospital, Chennai