From the Director’s Desk
November saw unprecedented rains bringing much needed relief to a parched city otherwise facing an imminent threat of drought. But the rains also wrought havoc on the city’s infrastructure, bringing activity to a grinding halt. The staff at Kauvery put in a laudable effort at maintaining uninterrupted, round-the-clock services in the face of extreme odds. We also organised Flood Relief Camps in affected areas like Kotturpuram and Saidapet, in association with Rotary Club of Madras East and Big FM.
The Department of Neurology at Kauvery organised two awareness programs in November. The ‘Epilepsy in Women’ program was conducted for our team of doctors at the hospital premises by Dr Prithika Chary, our Chief Neurologist on 24th November 2015. A program on Stroke Awareness for women was organized in partnership with Duchess Club at Hotel Savera on 26th November 2015 by Dr Prithika Chary & Dr Bhuvaneswari. At the program, 130 Duchess Club members were offered special stroke risk assessment packages.
Yet another interesting feature of this month’s bulletin is video talk on diabetic foot by Dr N Sekar, a leading Vascular Surgeon in the country. With foot-related problems becoming very common in diabetics, there is an urgent need for early and appropriate treatment, failing which this condition could lead to serious complications.
December is the beautiful month of Margazhi, the ‘Season’ when every street in Chennai comes alive with the sounds of classical music and dance. Situated at a stone’s throw from most of the leading Sabhas of Chennai, in the heart of this Margazhi utsavam as it were, we at Kauvery hope to catch the pulse of the Season and wish the citizenry a wonderfully satisfying celebration of the performing arts.
Dr Aravindan Selvaraj, MS Ortho, FRCS Ortho (UK & Ireland)
Executive Director & Chief Orthopaedic Surgeon, Kauvery Hospital
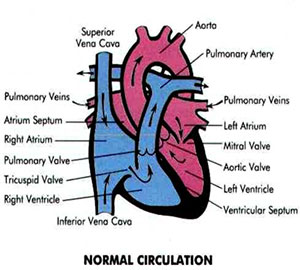
Know Your Child’s Heart
Article by Dr. R. Prem Sekar
Senior Consultant Interventional Paediatric Cardiologist, Kauvery Hospital, Chennai
Every year, at least 3 to 8 out of every 1000 babies are born worldwide with defective heart. In addition, a small proportion of children who are born with normal heart acquire heart conditions such as Rheumatic heart disease, Kawasaki disease, Myopathies etc.
Rheumatic heart disease usually follows a simple throat infection caused by the bacteria called beta-haemolytic streptococcus, which in some children damage the heart valves causing their malfunction.
Kawasaki disease starts as a fever, subsequently affecting the coronary arteries leading to complications such as heart attacks in children.
Myopathies are diseases of the heart muscle usually caused by some viral infections. The heart muscle weakens and becomes ineffective in its function as a pump, resulting in heart failure.
It is very important to suspect and diagnose these heart defects early. All these defects CAN be corrected with appropriate treatment. It IS possible for you to protect your children from these illnesses and help them live normal and full life.
1. Who is a paediatric cardiologist?
A Paediatric Cardiologist is a Children’s Heart Specialist who specializes in diagnosing heart diseases in children and offers solutions for normal life and growth.
2. When do parents need to take their children to a paediatric cardiologist?
• When either of the parents OR a previous child OR a close relative in the family has been diagnosed with a heart defect previously
• When the parents suspect that their child may have a heart problem
3. When should the parents suspect a heart problem in their child?
When the child shows any of the following symptoms:
As a baby: Breathing fast (tachypnoea), very slow interrupted feeding (suck-rest-suck cycle), sweating over the head while feeding (diaphoresis), poor weight gain (failure to thrive), going blue or dusky all over the body while crying (central cyanosis).
As an older child: Getting tired easily while playing (exertional fatigue), getting frequent chest infections (pneumonia), complaining of chest pain (palpitation), complaining of giddiness (syncope) and bluish discolouration (cyanosis).
4. How does the Paediatric Cardiologist check the baby’s heart?
The Paediatric Cardiologist checks the baby clinically for abnormal discolouration (cyanosis), abnormal pulse (rhythm disturbances and heart function) and abnormal heart sounds (murmurs). The common tests undertaken are Chest X-Ray (to see the position and size of the heart), ECG (to check the heart rhythm) and Echocardiography (to check for any structural problems in the heart and assess the heart function).
5. Can heart problems of babies be detected during pregnancy?
Yes, it can be done by using Foetal Echocardiography at 16-20 weeks of pregnancy. Elderly diabetic mothers, those with birth defects of the heart, and those who have previously given birth to babies with heart defects are advised foetal echocardiography.
6. What are the heart problems usually seen in children?
Heart problems in children may be CONGENITAL: these are defects at birth which are of two kinds – simple and complex.
Simple defects are those such as holes in the heart (ASD, VSD, PDA) and blocked valves (Aortic stenosis, Pulmonary stenosis, Coarctation of Aorta).
Examples of complex defects are blue baby conditions (TOF -Tetralogy of Fallot, TA -Truncus Arteriosus, TGA – Transposition of Great Arteries).
Heart problems in children may also be ACQUIRED: children have a normal heart at birth and then their heart becomes diseased (Cardiomyopathy, Rheumatic heart disease, Kawasaki disease).
7. Can these heart problems in children be cured?
About 95% of heart problems in children can be treated successfully. Majority of the simple problems can now be cured without operations by device closures and Angioplasty. Conditions cured without surgery are ASD, VSD, PDA, Coronary fistulas, Aortic stenosis, Pulmonary stenosis, Coarctation of Aorta. These procedures are carried out first by inserting small tubes called catheters into the heart through the blood vessels in the leg. Next with careful manoeuvres through the catheter, the holes in the heart are closed with devices; or the blockages in the heart are opened up with balloons and stents.
The advantages of these procedures are:
• complete cure of the heart without a visible scar on the body
• without blood transfusions
• without pain
• minimal hospitalisation period (usually 2-3 days)
• without a need for post-procedure resting period.
The complex blue baby conditions also have very good surgical solutions these days, providing the growing child with an excellent quality of life.
For more details on these procedures log on to www.hxplain.com
Management of Diabetic Foot
This video is about diabetic foot disease and why people with diabetes are losing their legs. There are blood vessels which carry good blood and ones which carry bad blood. The vessel which carries good blood is called artery. People with diabetes may develop blocks in the arteries of their legs resulting in gangrene which is death of the tissue. This is more common in people with diabetes, blood pressure, high cholesterol and in people who smoke or use tobacco in any form.
Talk by Prof N Sekar, MS, MNAMS, MCh (vascular), FICS, DSc (Hon.Causa), FRCS (Glasgow), Senior consultant vascular surgeon, Kauvery Hospital, Chennai.
Watch his video talk on YouTube.
Ask The Doctor
Doctor, why is it important that my child should be immunized?
Remember the old adage – “Prevention is better than Cure”? Well, immunizing your child is just that. There are certain diseases prevalent worldwide, especially in India, which can lead to dire consequences – even death. Diseases such as measles, diphtheria, mumps, polio, whooping cough, tetanus, rubella or German measles, Haemophilus influenza and rotavirus can all be prevented with vaccinations.
For instance, “Small Pox”, one of the most disfiguring diseases has been wiped off the face of our planet, thanks to the invention of an excellent vaccine. Immunizing your child helps not only protect your child effectively, but also prevent all the diseases named above.
Vaccines contain antigens that help the body produce antibodies to fight the disease causing germ. True, a vaccine contains in part the viruses or bacteria that cause the disease, but the immune system fights and destroys or weakens the viruses/bacteria, so that your children do not become sick. Children develop immunity through vaccinations and thus we, as parents, can help protect our children from contracting the actual disease.
Here are a few more facts why immunization is important.
- A newborn baby is immune to many diseases as the baby has got the necessary antibodies from mother. The immunity, however, is effective only for the duration of the first year of life.
- Prior to the advent of vaccinations, many children died from diseases such as measles, polio, and whooping cough. An unvaccinated child exposed to any of these diseases is not usually strong enough to fight the disease. Immunization with proper and timely vaccinations gives the baby better protection and a better fighting chance against these harmful diseases.
- Diseases caused by failure to administer vaccinations lead to frequent visits to the doctor, hospitalization, loss of time, dislocation of work, avoidable medical bills and in some cases premature death.
- Immunization of every child assures a healthy and wealthy future of the nation, as health is the real wealth.
Doctor, I have heard about the harmful impact of Meningitis. Could you give me a clear picture of this illness?
Meninges are the three membranes that cover and protect the brain and the spinal cord. Meningitis is the inflammation of the meninges caused by injury or infection. There two types of meningitis: the first is caused by a virus and the second by bacteria, the latter being the more virulent. Infections caused by viruses most often get better on their own, but if infected by bacteria, it is very important to seek treatment immediately. Bacterial meningitis can cause death or brain damage unlike viral meningitis.
In addition to the viral and bacterial types, meningitis can also be caused by the following triggers:
- Parasites
- Fungi
- Chemical irritations
- Tumours
There are many types of viruses which can cause meningitis, some of which include:
- Enteroviruses (which cause intestinal illnesses as well)
- West Nile Virus – spread by a species of mosquitoes causing viral meningitis
- Mumps and HIV viruses – cause a type of meningitis called aseptic meningitis
- Herpes virus – causes Herpes meningitis. This is the same type of virus that causes genital herpes and cold sores, though people with cold sores or genital herpes do not necessarily develop meningitis.
Late summer, into the East Monsoons is generally the time when viral meningitis may occur. Children and adults under the age of 30 are the most vulnerable to an attack of viral meningitis.
Symptoms to watch out for:
- Severe headache
- Fever and shivers (particularly in children and newborns)
- Agitation
- Changes in mental status
- Photophobia
- Meningismus (stiff neck)
- Vomiting and Nausea
- Decreased alertness
- Rapid breathing
- Head and neck arched backwards
- Bulge in the fontanelles in babies (soft spot on the skull)
If you observe one or more of these symptoms, or suspect that it could be an attack of meningitis, then consulting a doctor immediately and seeking urgent medical treatment is very important.
Removal of Gallbladder by Laparoscopy
The Gallbladder is a small organ located under the liver. Its purpose is to store the extra bile produced by the liver, and secrete it to the small intestines, where the bile aids in the digestive process. The bile is a fluid and is composed of:
- Cholesterol
- Bile Salts
- Bilirubin (an orange-yellow pigment in the bile formed as a breakdown product of haemoglobin)
The bile thus helps digest the fat in the food that is consumed.
Gallstones that are formed in the gallbladder can happen due to several reasons, such as genetics, reduced motility in the gallbladder, diet and body weight. There are two types of gallstones:
- Cholesterol stones: In 80% of the cases, the gallstones are of this type. They are greenish yellow in colour. The cholesterol stones form when there is too much cholesterol in the bile. Another reason for cholesterol stone formation is attributed to the inability of the gallbladder to empty itself quickly.
- Pigment stones: Made of bilirubin, these stones are smaller in size and darker in colour. These stones are more common in people with certain medical conditions like cirrhosis of the liver, and blood disorders such as sickle cells or anaemia.
Risk factors for developing gallstones
- Hereditary factor: Anybody with a family history of gallstones is at risk.
- Uncontrolled weight/obesity: Being one of the biggest risk factors, obesity can cause rise in the cholesterol levels in the bile, which prevents the gallbladder from emptying itself.
- Estrogens: High levels of estrogens too can reduce motility in the gallbladder. Pregnant women and those who have undergone hormone replacement therapy are at greater risk.
- Gender and age: Women and elderly people are more prone to develop gallstones.
- Cholesterol Medications: A few types of cholesterol-lowering medications can increase the amount of cholesterol in the bile, thus increasing the possibility of developing gallstones.
- Weight Loss and Fasting: Losing weight rapidly causes increased levels of cholesterol formation in the bile, which in turn causes the development of gallstones. Fasting causes the gallbladder to contract less, thereby increasing the chances of gallstones formation.
- Diabetes: Diabetic people tend to have a higher level of triglycerides in their blood. This is a big risk factor for formation of gallstones.
The Procedure
Laparoscopic gallbladder removal surgery or cholecystectomy is a very safe and effective procedure. There are very low risks involved in this surgery.
The surgeon makes four small (keyhole size) openings in the abdomen. A laparoscope with a lighted scope attached to a camera is inserted into the incision closest to the belly button. The surgeon uses a video monitoring screen for guidance while inserting the surgical instruments through the remaining incisions, to remove the gallbladder. Prior to removing the gallbladder, a special X-ray procedure called intraoperative cholangiography may be performed to view the anatomy of the bile ducts.
Anaesthesia
General anaesthesia is administrated prior to the procedure.
Post Laparoscopic Surgery
- The recovery time is very quick. You may be required to stay in hospital for 3-4 days.
- The bile will flow directly from the liver to the small intestine and will not affect the digestive process.
- Some discomfort maybe there for a week, but 10 days (normally), after the procedure, you will be able to resume all normal activities.
- No special diet is required.
Events of the past month
Kauvery Hospital organized Flood Relief Camps in the city and lots of people benefitted.
“There are at least four things you can do with your hands. You can wring them in despair; you can fold them in idleness; you can clench them in anger; or you can use them to help someone”
Hundreds of people benefitted in Flood relief camps organized in RA Puram, Kotturpuram, Saidapet and Nehru Stadium recently. Free medicines were distributed along with free treatment.
Stroke Awareness Program
Stroke Awareness Program by Kauvery Hospital and The Duchess Club was conducted at Savera Hotel on 26/11/2015. The program was organized by Dr.Prithika Chary, Chief Neurologist and Neuro Surgeon and Dr.Bhuvaneswari, Consultant Neurologist, Kauvery Hospital. A special stroke risk assessment package of Rs.6000 was given to all.
Epilepsy in Women
“Epilepsy in Women” a program for doctors and nurses was held at Kauvery Hospital on 24th November 2015. The program was conducted by Dr. Prithika Chary, Chief Neurologist, Kauvery Hospital.
Pediatric Cardiac Camp
A Pediatric Cardiac camp was conducted at Mettupalayam on 11/11/2015. 140 kids with cardiac issues were screened by Dr. Prem Sekar, Senior Consultant Pediatric Cardiologist, Kauvery Hospital.
Upcoming Events
General Medical Camp at Mahindra City, Chengalpattu
Kauvery Hospital will conduct a general medical camp for employees of NCR Systems Pvt Ltd at Mahindra City, Chengalpattu on 01/12/2015.
Time: 10 AM – 4 PM
Adult and Paediatric Cardiology Camp in Kumbakonam
Kauvery Hospital in association with AIWA will hold an adult and pediatric cardiology camp at Kumbakonam on 05/12/2015.
Time: 9 AM – 2 PM
One Day CME [C- KRAC]
A One day CME for doctors and PGs’ on regional Anesthesia will be conducted by Kauvery Hospital at Crowne Plaza, Chennai Adyar Park on 13/12/2015.
Time: 8 AM – 6 PM
Cardiology Camp at Vellore
Kauvery Hospital will conduct a Cardiology camp at Vellore on 13/12/2015.
Time: 9 AM – 2 PM
Cardiology Camp at Adambakkam
Kauvery Hospital will organize a Paediatric Cardiology camp at Adambakkam during the 2nd week of December 2015.
Time: 10 AM – 2 PM
Cardiology Camp at Velachery
A Cardiology camp at AABIAH Clinic Velachery will be organized by Kauvery Hospital during the 2nd week of December 2015.
Time: 10 AM – 2 PM
Ortho and General Camp at Perungudi and Guindy
A 5-day Ortho and general camp will be conducted by Kauvery Hospital for employees of Verizon System at Perungudi and Guindy campuses.
Date & Time: TBA
Patient Experience
“We had an excellent consulting experience & treatment from Dr. Amal Louis & Dr Prithika Chary. Dr. Amal Louis advised us & explained the treatment & the procedure planned. Special thanks to nursing team (Vinnarasai, Bency, Roopa, Sowmya, Papitha and CCU nursing sister Nagalakshmi) who were all very pleasant and helpful. Overall a very good experience with no complaints.”
– K.S
“Helen from PALS department was very helpful. Her calm composure and smiling face brought a lot of warmth entire team was friendly and responsive. Thank you Kauvery Hospital.”
– R.S
“We are very grateful that we had access to this hospital for my mother. Very good experience and all the services were very good. A special word for the nursing team who went out of the way to be sensitive and attentive.”
– P.B
“The hospitality of the staff & nursing are examples for excellence and I would like to appreciate each and every resource personally. I wish the same standard should be maintained throughout. if this sort of service continues this will be India’s number one hospital.”
– N.B
“Very courteous & friendly. Quiet good response from all doctors and nurses.”
– B.G
“Caring and helpful staff. Hospital is very neat and clean. Very good service. Keep up the good work!”
– J.S
“Very good hospital staff and assistance. Good guidance by doctors. I am very happy.”
– D.K
“I am very very happy about your service and your valuable support and co-operation for my wife and her recovery I really appreciate for your support.”
– S.S
Recipe Corner
Punjabi Chole
This yummy, authentic Punjabi Chole recipe has the flavors and bite of Punjab rolling off your tongue. Chole can be made in several different ways, but there is nothing to beat the taste of the original Punjabi Chole dish. This dish is a hot favorite at all Punjabi Dhabbas (roadside restaurants) and restaurants that serve à la carte, too.
Serves: 6; Calories per serving: 244.7
Nutritional Value: Chick Peas, Garbanzo beans, Kabuli Channa or Punjabi Chole is high in dietary fiber, with moderate Carbohydrates, low fat content, rich in Vitamin A, B6, B12, C, D and E, and has zero Cholesterol. Total Fat 6.7g; Sodium 767.9mg; Potassium 561.2mg; Protein 6.9g, Carbohydrate 42.6g, Dietary Fiber 6.7g; other minerals present per serving include calcium, copper, magnesium, manganese, iron, selenium, thiamin, phosphorus, folate and riboflavin.
Ingredients:
To Pressure Cook
- Chickpeas (Kabuli Channa, Chole, or garbanzo beans) 250 gms / ¼ Kg
- Salt ½ tsp
- Black tea bag 1 or dried Amla (gooseberry)
- Water 3 cups or 750 ml
For Gravy
- Red Onion medium-sized 1, finely diced
- Apple Tomato medium-sized 1, finely chopped
- Garlic cloves 3 small, finely diced or ground to a paste
- Fresh ginger ½ inch piece (ground to a paste)
- Turmeric Powder ¼ tsp
- Red Chili Powder ½ tsp
- Amchur or Mango Powder ¾ tsp
- Pomegranate powder ½ tsp
- Green Chilies 4, slit
- Curd or plain Yoghurt 250 ml
- Refined oil 3 tablespoonsv
- Salt to taste
Spices (to be ground separately)
- Black Cardamom 2
- Cinnamon 1 inch
- Peppercorns 4
- Cloves 2
- Indian Bay Leaf 1 medium size
- Carom Seeds or Omum ¼ tsp
- Cumin Seeds or jeera 1 tsp
- Coriander seeds or Dhania 1 tsp
- Fennel Seeds or Saunf 1 tsp
- Dry Red Chilies 2
For Garnishing
- Fresh Green Coriander leaves, coarsely chopped
- Fresh ginger ½ inch, julienned
- Red onion 1 medium size, sliced in circles or chopped
- Tomato 1 medium size, chopped or sliced or cut; use smaller tomatoes to create flower shapes if inclined to decorate
- Lime 1, quartered or slices/wedges
Preparation:
1. Rinse and soak the chickpeas in plenty of water in a large bowl. Soak the chickpeas either overnight or 8 hours before making the Chole. Chickpeas absorb water and bloat in size, so soak the chickpeas in a good amount of water.
2. To lend color to the chickpeas or channa, add a piece of dried amla (gooseberry) or one bag of black tea. This adds additional flavor to the channa stock.
3. Place a pressure cooker atop the stove, light the fire to medium high. Put the soaked chickpeas, together with water, 3-4 pieces of dried amla (or the black tea bag) into the pressure cooker. Add just sufficient water to cook the chickpeas/channa.
4. Season with salt and pressure cook the chickpeas for 20 to 30 minutes (the chickpeas must be soft).
5. Next place a Kadai or saucepan on the stove, on low flame. Dry roast the spices, to medium brown. Do not blacken the spices or this will change the color of the Chole. Ensure stirring continuously as you roast the spices.
6. Switch off the flame and allow the roasted spices to cool down first, and then transfer them to a dry grinder/blender.
7. Place a sauce pan or kadai on the stove, on low flame. Add oil to the sauce pan/kadai and heat.
8. Add the finely diced onions to the oil and sauté, until light brown in color.
9. Add the ginger paste and chopped garlic (or garlic paste) and sauté, until the raw smell fades away.
10. Next add the chopped tomatoes and sauté until they are soft or until the oil begins to bubble out.
11. Once the tomatoes are cooked, add in the turmeric powder, chili powder, and salt (just enough for the masala, as salt has already been added to the chickpeas). Stir till the powders lose their raw smell and the oil bubbles up from the masala.
12. Stir in the dry ground masala powder and sauté, till the oil once again rises.
13. Remove the amla pieces or tea bag from the cooked chickpeas, drain the stock out. Add the cooked chickpeas or channa to the masala in the saucepan and stir the gravy in well and allow to simmer for 5 minutes.
14. Add in the cup of curd or yoghurt together with the split green chilies and stir well. Close the pan with a lid and allow the mix to simmer for about 5-10 minutes.
15. Finally add in the amchur powder and pomegranate powder and stir, simmer for another minute or two. The gravy will now be thick.
16. Garnish with the chopped coriander leaves.
17. Decorate with raw onion rings and tomato flowers (or just chopped onions and tomatoes).
This dish can be served as a side dish with Curd Rice, Lemon Rice, or can be eaten with Chappatis, Parathas, Rotis and Pulkas. It tastes best with Pooris and Baturas.