Diabetes Mellitus and Neurology
Diabetes mellitus is a chronic disease that occurs either when the pancreas does not produce enough insulin (a hormone that regulates blood glucose) or when the body cannot effectively use this insulin. There is an explosive increase in the incidence of diabetes globally. The incidence is more in South Asian countries including India. India is now referred to as the DIABETIC CAPITAL of the world. Almost 50% of Indians in the age group of 50-60 years are either diabetic or prediabetic.

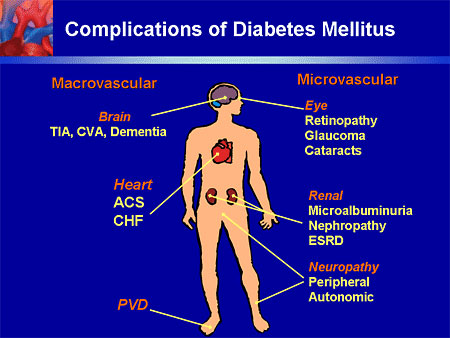
Diabetes is a disease with effects on multiple organs in the body. Poorly controlled diabetes can affect your body from top to toe: brain, heart, abdomen, kidneys and nerves.
The prevalence of neurological complications in diabetes is almost 50%, of which peripheral neuropathy is 27.5%. Neurological complications of diabetes are multiple and varied, they include:
- Peripheral neuropathy
- Diabetes-related retinal disease and cataracts leading to blindness
- Strokes – Both due to both blood clot and bleed
- Autonomic disturbances like urinary retention or incontinence, abnormal gastro-intestinal movements causing bloating, constipation or loose stools
- Cranial nerve involvement causes double vision or facial weakness
- Cognitive dysfunction like vascular dementia
Diabetes-related peripheral neuropathy is a very common problem that doctors come across. This complication is mainly due to the fact that diabetes is a metabolic problem with faulty utilisation of glucose and this faulty mechanism releases toxic substances such as O2 radicles, ↑sorbitol, etc., which cause damage to the nerves over time. Vascular supply to the nerves is also compromised in diabetic patients, contributing to nerve damage.
Clinical Presentation
Patients having diabetic neuropathy will have the following symptoms and signs. Diabetic neuropathy could also be the heralding feature leading to the diagnosis of diabetes mellitus in many patients.
Patients with peripheral neuropathy usually complain of the following symptoms and signs
- Burning pain mainly in the feet and hands
- Sometimes abnormal skin sensations such as tingling or pins and needles
- Pain is more severe during nights
- Increased sensitivity to pain (hyperalgesia)
- Pain to non-painful stimuli (hypoesthesia)
- Reduced ability to differentiate hot from cold
- Glove and stocking distribution of numbness
- Loss of balance
- Muscle weakness
- Non-healing foot ulcers, hammertoes, etc.
Diabetic Neuropathy is Broadly Classified into 3 Types
Sensory Neuropathy: Mainly affecting the sensory or feeling nerve fibres.
- Most common type
- Characterized by numbness, pain, burning/prickling sensation and glove and stocking distribution of numbness
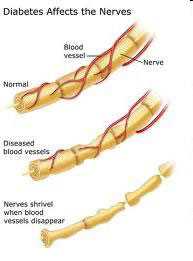
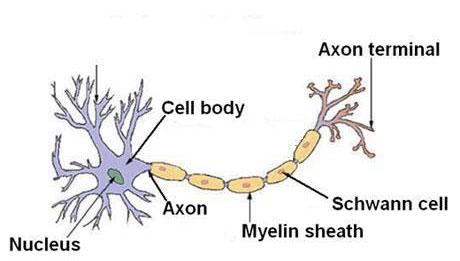
Motor Neuropathy: Mainly Affecting Nerve Fibres Supplying the Muscles
- Very rare form
- Characterized by muscle pain and weakness
Autonomic Neuropathy
- Nerves controlling involuntary activities in body are affected.
- Nerves in cardiovascular, gastrointestinal, genitourinary and sweat glands may be affected.
- Characterized by diarrhoea, symptoms of gastro paresis like feeling of stomach fullness, vomiting and abdominal bloating, constipation, urinary incontinence or urinary retention, impotence in men, blood pressure fluctuations causing syncope or fainting.
Diagnosis
Patients with signs and symptoms suggestive of diabetic neuropathy should seek medical care ASAP. Diagnosis is made following a thorough clinical examination and some laboratory tests including fasting and post-prandial glucose and HbA1c indicating your long-term DM control and blood tests to rule out other causes such as vitamin deficiencies, thyroid and toxic substance misuse. Tests for vascular parameters, for e.g., Dopplers and ankle-brachial index are also indicated.
Imaging such as ultrasound or MRI of the nerves in select cases.
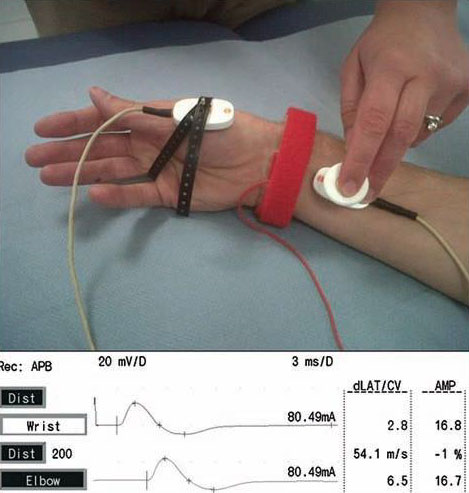
However, the most important test in the diagnosis of peripheral neuropathy is nerve conduction studies (NCS).
Thus, confirmation of diagnosis by NERVE CONDUCTION studies is necessary and it gives us information regarding the nerve affected, the pattern of neuropathy and its severity.
Treatment
Treatment mainly aims at controlling the symptoms, slowing the progression of neuropathy and early identification and treatment of its complications.
Acute onset neuropathy can be cured with immune-modulatory drugs in some patients but in patients with chronic neuropathy, the treatment is mainly symptomatic with great effect.
Good Glycemic Control
- Tight and stable glycemic control is probably the most important for slowing the progression of neuropathy.
- The Diabetes Control and Complications Trial (DCCT) demonstrated that tight blood sugar control in patients with type-1 diabetes decreased the risk of neuropathy by 60% in 5 years.
Physical Measures
- Walking
- Foot care and right foot-wear
- Physiotherapy
- TENS/Ultrasound therapy
- Smoking cessation, cut down alcohol
Medications
There are several medications used for symptomatic control of the signs and symptoms of neuropathy such as pregabalin, gabapentin, carbamazepine and sodium valproate, opioids for pain management.
Topical therapy with capsaicin or transdermal lidocaine.
Vitamin supplementation with zinc sulfide showed improvement in glycemic control and certain B vitamins reduce paresthesia or symptoms of neuropathy.
Foot ulcers can be a major complication in patients with diabetes and peripheral neuropathy.
They are managed with foot care, protective and customised footwear and antibiotics if infection is present.
Surgical treatment if there is a severe infection or blood supply compromise.
Most complications of diabetes are preventable with healthy lifestyle habits and some can even be reversed. Taking steps to prevent and control diabetes doesn’t mean giving up on sweets completely. Eating healthy food is important. Carbohydrates have a big impact on blood sugar levels than proteins and fats.
So, a good lifestyle with moderate exercises such as walking, a balanced diet and good sugar control can pave the way for a long and healthy life.

Dr. Bhuvaneshwari Rajendran
Senior Consultant, Neurology and Clinical Neurophysiology
Kauvery Hospital, Chennai

