Technological Transformation pushing New Frontiers in Neurosurgery
My journey as a neurosurgeon began 20 years ago. After completing my specialization in Neurosurgery, I went through training and apprenticeship with senior surgeons before becoming an independent surgeon, a teaching faculty and a senior neuro surgeon.
The one aspect that has endured throughout my neurosurgical career, is my fascination with Technology, or with what I call the interface between today and tomorrow. The fascination started right from the time I had to use an operating neuro microscope as a student and through all the various fine and delicate instruments and technologies, I have seen evolve and being used.
Technology – the real game-changer in Neurosurgery
Technology is a great leveller. Today, Indian hospitals carry medical equipment that is on par with top hospitals of the world. Medical Technology is erasing the East-West or North-South divide between (rich and poor) nations. In the process, citizens of most countries now have access to similar standards of healthcare.
Like with any other industry, Medical Technology too has been shaped by technology paradigms that disrupt our lives from time to time. In the last 3 decades, the Internet, the Mobile revolution, Social Media, Analytics, Cloud Computing, Artificial Intelligence (AI), Robotics and 3D Printing have all influenced innovations in Medical Technology as well.
So let us examine how new and emerging technologies have changed, or is changing neurosurgical care worldwide.
Neuro-navigation
Neuro-navigation is a fascinating confluence of Imaging and Image Integration that aids Real-time Surgical Visualization. This technology helps surgeons locate, remove or conduct intervention in delicate areas of the brain and Spine, bringing in more precision than before. Neuro-navigation to a neurosurgeon is what GPS means to a driver. This is the evolution of Minimally Invasive Surgery (MIS).
Neuro-navigation takes MIS to the next level. Here, even as the surgeon is looking at the area to be operated under microscope, his surgical vision can be superimposed with an scan image of the lesion in that area. Or it can be displayed on a screen. Then, the GPS- like system tells the surgeon exactly where his/her instruments are, with reference to the above scan image. This way, the surgeon is guided through the operating area, so that he/she can remove a tumour, or fix a screw (as in the case of spinal surgery), with pin-point accuracy. This eliminates unnecessary incision size and the resultant blood loss.
Kauvery Hospital has acquired such a state-of-the-art Neuro-navigation system and we are privileged to provide this service.
Robotics
Robots are already assisting surgeons in specialties like urology, surgical gastroenterology and radiotherapy. Now they have made a foray into Neurosurgery as well.
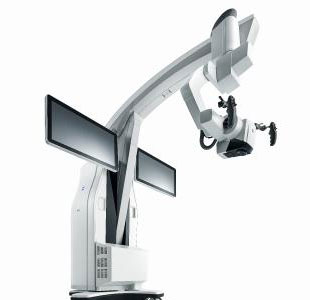
In the area of Neurosurgery, the combination of robotic intervention and neuro-navigation, as described above, is used for high-precision surgeries. Surgeries like that of the spine are delicate and involve fine manoeuvring through layers of bone, muscle tissue and nerves. The robotic arm acts as an extension to the surgeon’s arms and undertakes delicate interventions guided by the surgeon, who is in turn guided by the image he/she is seeing on a screen. The robot can make very subtle movements required for precise interventions, never deviates from the track and if moved accidentally redirects itself back to the desired position (thanks to intelligence built into its hardware and software).
This kind of a procedure is invaluable in Deep Brain Simulations that is part of the therapy for conditions like Parkinson’s disease.
Robotic microscope is integrated to the Neuro-navigation, where even a slight deviation from the target of surgery is auto-corrected by the microscope. In other words, even the slightest movement of the microscope by the neurosurgeon wouldn’t in anyway allow loss of focus from the target lesion.
Kauvery Hospital has now deployed a Robotic Neuro-microscope which is a boon for our patients undergoing precision neuro surgery.
3D Printing
Tumour surgery or functional surgery for correcting movement disorders such as Parkinson’s disease or Epilepsy involve several steps and require careful planning, Till recently, such planning was done on paper, computers or in face-to-face discussions between members of the surgical team.
Now, such planning can be simplified using 3D Printing. Using a 3D Printer, surgeons can create replicas of the patient’s brain, spine or organ to be operated. The tumour or deformity can also be simulated through the model. The surgical team can then plan the surgery by dissecting the 3D printed model as if they were performing the surgery. The model acts as a blueprint and can be as intricate as desired, replete with blood vessels, muscle tissue, etc. 3D printing is a priceless technology to recreate lost bones of the skull and face or to replace them when damaged.
In The Not Too Distant Future…
The confluence of Neuro-navigation, Robotic intervention and Artificial Intelligence opens up the possibility of having Robotic Moderators in ICUs or Robotic Assistants in Operating theatres.
3d printing in this future time would possibly create neuro-prosthetics that replace biologically or stem cell derived specific neurons or entire brain Spinal cord portions revolutionizing neurosurgical treatment like never before.
Telesurgery
There are many surgeries which are routine in nature and have the same sequence, with very little deviation from the plan. Such surgeries in the future will be performed remotely without the surgeon present in the OT.
The concerned surgeon can organize the surgical team involving nurses, junior doctors and a Robotic Surgical Assistant. Through the Internet, the real surgeon can see a 3D image of the patient’s operating area. The robot has arms and built-in AI protocols to carry out the surgery on its own, with little to no intervention from the remote surgeon who is supervising the surgery.
Nano technology
Nano technology and its applications like nano-instruments, nano-drugs and nano-implants can revolutionize the neurological landscape like never before. A nano instrument or a nano-robot can enter the sub-cranial space, and crawl deep into the crevices of the brain, removing tumours with high precision, or correcting some deformity, as it moves. The nano-robot can expand or shrink in size as required to complete the intervention.
This opens up possibility of a patient going to sleep, during which the nano-robot enters his/her body, performs the intervention and exits the body. He/she then wakes up with the tumour gone.
Cyborgs
Cyborgs may be the stuff of science-fiction movies today, but in 50 years’ time, they could become a reality. Stem-cell research is helping doctors replicate parts of organs and implant them into the patient’s body so that the organ can heal itself. Cyborgs are the natural evolution of stem-cell therapy and all the technologies described above. An IC chip which has all the intelligence required to move a particular limb or organ is implanted in the brain, so that the brain is able to control an artificial limb or organ, as it would a real one.
An AI-driven artificial brain or its robotic clone can be replete with all the chips required to control various functions and organs of the body, be they natural or stem-cell-developed clones. The chips can even factor the various layers of human intellect while memory chips can carry the history of the individual, so this way, a cyborg with a distinct identity can be created.
This way, parts of the human brain can be cloned, in order to overcome movement disorders, brain tumours, or even the effects of ageing.
Conclusion
The new frontiers of Medical Technology, as applied to Neuroscience, bring up legal and ethical issues about rights, relationships, decision-making and human identity, as they would practically make humans immortal. However, as with every new technology paradigm, these technologies too would get regulated with time, so that their application is more rational and conforms to the framework of human existence as we understand it.

Article by Dr. Shyam Sundar Krishnan
Senior Consultant – Brain and Spine Surgeon
Kauvery Hospital

