From elective surgery to mechanical ventilation: A critical post sterilization nursing care
Deepa. S1*, Subathra Devi M2, Maha Lakshmi3
1Nursing Supervisor, Kauvery Hospital, Cantonment, Trichy, Tamil Nadu
2Nurse Educator, Kauvery Hospital, Cantonment, Trichy, Tamil Nadu
3Nursing Superintendent, Kauvery Hospital, Cantonment, Trichy, Tamil Nadu
*Correspondence
Abstract
Female sterilization is a commonly performed elective surgical procedure with minimal expected morbidity. However, rare and unexpected postoperative complications can result in rapid clinical deterioration. This case report describes a reproductive age woman with a history of self-administered medical abortion one month prior to admission, who later underwent elective sterilization at an outside hospital. In the post-operative period, she developed fever and progressive respiratory distress and was referred to tertiary care. On arrival she required immediate mechanical ventilation due to prolonged ventilation tracheostomy being performed. Despite aggressive intensive care and comprehensive nursing management, the patient succumbed to illness. This case emphasizes the importance of vigilant postoperative monitoring early recognition of deterioration and life-threatening respiratory compromise.
Key words: Female sterilization; Contraception; Respiratory distress
Background
Female sterilization is a widely used permanent method of contraception and is generally considered a safe elective surgical procedure with minimal complications. However, in rare situations patients may develop unexpected postoperative symptoms requiring immediate medical attention. This report highlights the importance of early recognition of clinical deterioration and the critical role of nurses in providing timely monitoring and supportive care in patients requiring intensive care management.
Introduction
Female sterilization is a commonly performed permanent contraceptive procedure and is generally considered safe with minimal complications. However, rare postoperative complications may occur and require prompt medical attention. This report describes a patient who developed fever and severe respiratory distress after sterilization requiring intensive care management including intubation, tracheostomy, highlighting the importance of nursing care in early recognition and management of critically ill patients.
Case Presentation
A 34‑year‑old female, P2L2, was admitted to an outside hospital on 01/02/2026 for a sterilization procedure and underwent surgery on 04/02/2026. She received two units of blood transfusion there in view of anemia. Later, during her hospital stay, she developed shock and dyspnea and was referred to our hospital with inotropes support.
Social History: She does not have any social history of drug addiction.
Allergies: No known medicine or environmental allergies
Past Medical History: No past medical history.
Past Surgical history: No past surgical history
Physical Examinations
On arrival at our emergency room, her sensorium was irritable and restless, she was tachycardic, tachypnoeic, hypothermic, and had peripheral cyanosis
Vitals
| PR | 142/min |
| BP | 60/40mmHg |
| Temp | 98'F |
| SpO2 | Not Recordable |
| RR | 44/min |
| GCS | E4 V4 M5 |
| CVS | S1S2 (+) |
| RS | BAE (+), bilateral NVBS (+) |
| P/A | Soft, tenderness (+) |
Markable Investigation
| S. No | Investigation Name | Result |
|---|---|---|
| 1 | Beta - Human Chorionic Gonadotropin (Beta - HCG) | 277.00 mIU/mL |
| 2 | Bicarbonate | <10.0 mEq/L to17 mEq/L |
| 3 | Blood Group and Rh Type - Automated | O Negative |
| 4 | CA++(7.4) | 0.82 mmol/L to0.90 mmol/L |
| 5 | Chloride | 99 mmol/L to107 mEq/L |
| 6 | Control (PT) | 11.7 Seconds |
| 7 | Creatinine | 5.7 mg/dL+4.6 mg/dL |
| 8 | Dengue Antibody IgM | Negative (0.69) |
| 9 | Dengue NS1 Antigen | Negative (0.82) |
| 10 | Direct Bilirubin | 10.8 mg/dL+23.9 mg/dL |
| 11 | Fibrinogen | 108 mg/dL+146 mg/dL |
| 12 | Gamma - Glutamyl Transferase (GGT) | 238 U/L |
| 13 | Haematocrit | 27 %+21 % |
| 14 | Haemoglobin | 8.2 g/dl+7.3 g/dl |
| 15 | Hepatitis B Surface Antigen (HBsAg) | Negative (0.12) |
| 16 | Hepatitis C Antibody (Anti HCV) | Non-reactive (0.01) |
| 17 | INR | 1.66. |
| 18 | Lac | 10.4 mmol/L+5.1 mmol/L |
| 19 | Lactate Dehydrogenase (LDH) | 3401 U/L+2125 U/L |
| 20 | Magnesium | 3.0 mg/dL |
| 21 | NA+ | 128 mmol/L+137 mmol/L |
| 22 | PCO2 | 30 mm Hg+41 mm Hg |
| 23 | pH Blood | 7.05 NA+7.18 NA |
| 24 | Phosphorous | 11.0 mg/dL |
| 25 | Platelet Count | 27000 cells/µl |
| 26 | Potassium | 4.2 mmol/L+6.9 mmol/L |
| 27 | Procalcitonin | >100 ng/mL |
| 28 | Pus cells | 6-8 |
| 29 | Scrub Typhus IgM Antibody | Negative |
| 30 | Sodium | 131 mmol/L+139 mmol/L |
| 31 | Test (PT) | 19.2 Seconds+ 15.4 Seconds |
| 32 | Total Bilirubin | 11.9 mg/dL+25.1 mg/dL |
| 33 | Total Protein | 4.8 g/dl+6.3 g/dl |
| 34 | Total RBC Count | 3.96 ML/10^9+2.96 ML/10^9 |
| 35 | Total WBC Count | 34880 Cells/Cumm+7720 Cells/Cumm |
| 36 | Troponin I (Quantitative) | 3.35 ng/mL |
| 37 | Urea Serum | 104 mg/dL+284 mg/dL |
Abdomen Scan Report – Bedside (06.02.2026): Mild thickened endometrium
Echocardiogram (06.02.2026)
- Normal chambers dimension
- Global hyperkinesia of LV
- Severe LV systolic dysfunction
- Grade I LV diastolic dysfunction
- Mild MR
- Mild TR / Mild PAH
- Septate intact
- No pericardial effusion / Clot
- Tachycardia noted during study (HR: 121bpm)
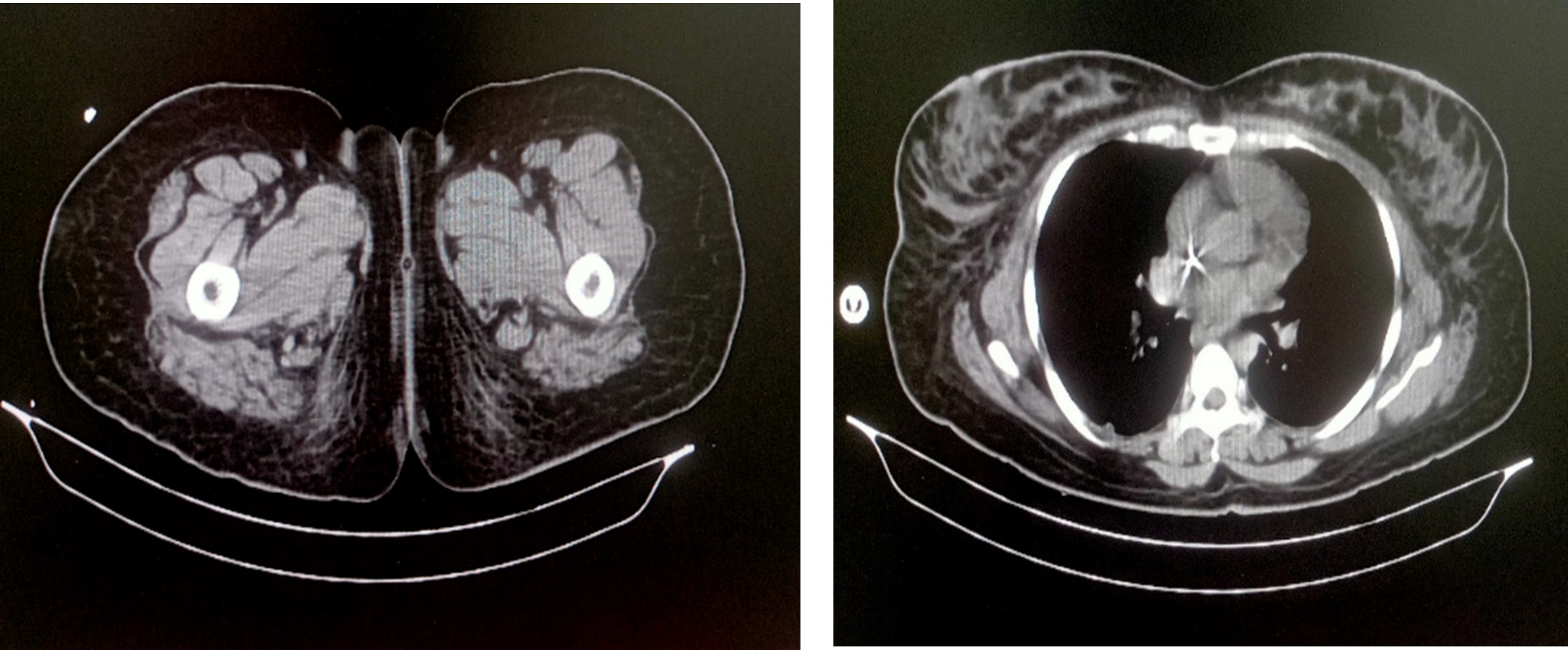
Multislice CECT -Abdomen and pelvis (06.02.2026)
A case of post sterilization, CECT abdomen showed:
- Bulky left rectus abdominis muscle and intramuscular hematoma with active bleeding
- Bilateral renal cortical necrosis
- Minimal hematoma on the left side of pelvis
EEG Report (11.02.2026)
This EEG record suggests diffuse cerebral dysfunction.
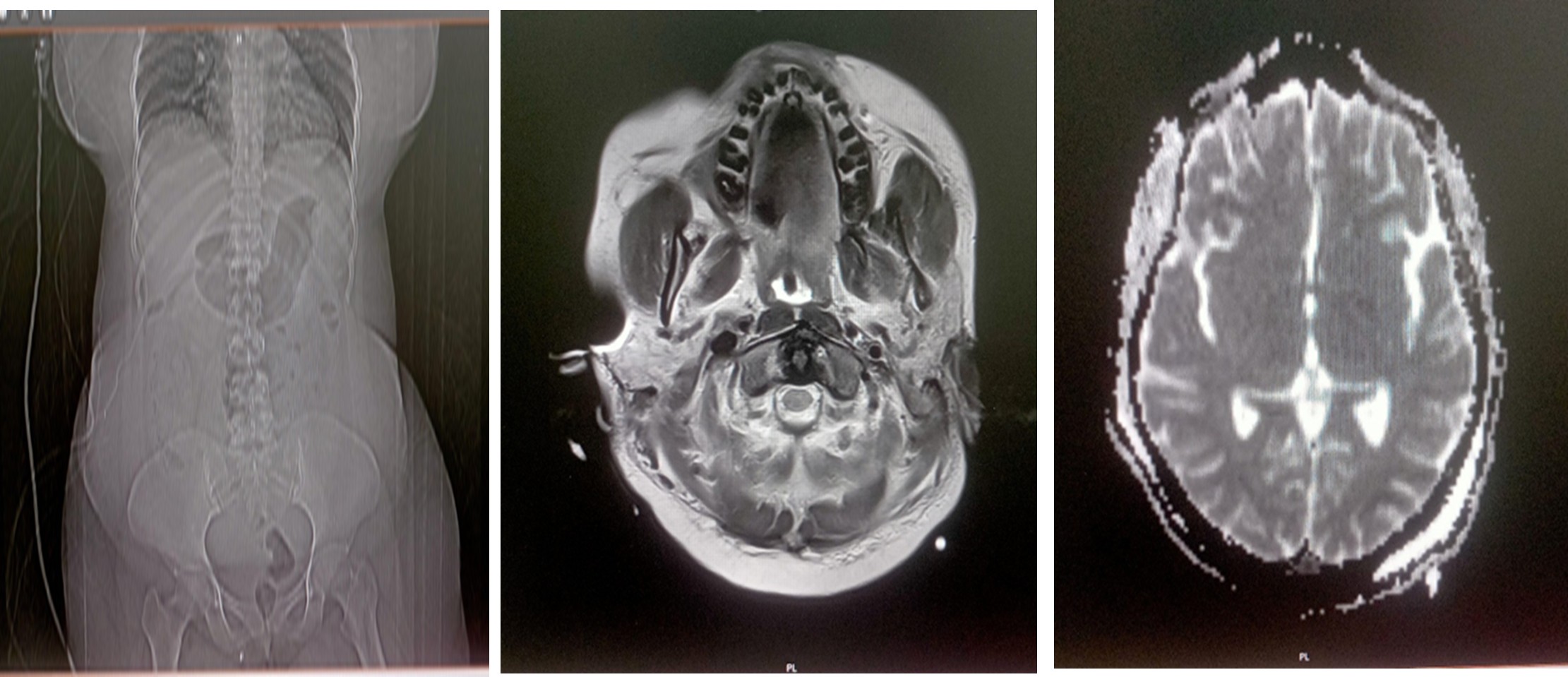
MRI Brain Plain Report (14.02.2026)
T2/Flair hyperintensities bilateral thalami with patchy areas of diffusion restriction? Hypoxia.
Abdomen Scan Report – Bedside (07.02.2026)
- Well defined heterogeneous collection in left rectus abdominis muscle – Likely hematoma
- No significant increase in size compared to CECT scan dated on 06.02.2026
- Bulky uterus
- Minimal ascites
- Left minimal pleural effusion.
Diagnosis
- Sepsis of unknown origin with multiorgan dysfunction
- Recent post sterilization status
- DIC / severe thrombocytopenia
- AKI/ renal cortical necrosis on HD
- Severe septic shock
- ARDS
- Stress cardiomyopathy – severe lv dysfunction
- Hypoxic ischemic encephalopathy
- Acute liver injury
- Prolonged weaning – post tracheostomy status
- Ventilator associated pneumonia.
Management and Treatment
On arrival at our emergency room, her sensorium was irritable and restless; she was tachycardic, tachypnoeic, hypothermic, and had peripheral cyanosis that was more in the right upper limb. Saturation was not recordable and her blood pressure was 60/40 mm Hg. Necessary laboratory investigations, including cultures, were sent. Bedside ultrasonography with echocardiography showed good left‑ventricular contractility with a collapsed inferior vena cava. Treatment was initiated with non‑invasive ventilation, broad‑spectrum antibiotics (Meropenem), adequate intravenous fluid resuscitation, inotropes, antipyretics, and other supportive measures. Arterial blood gas analysis revealed severe metabolic acidosis with high lactate levels. After initial stabilization with IV fluids and inotropes BP improved, saturation stabilized with NIV. The patient was shifted to the ICU for further management. Initial laboratory investigations showed severe anemia, elevated procalcitonin, leukocytosis with severe thrombocytopenia, and deranged renal and liver function tests. Contrast‑enhanced CT of the abdomen demonstrated bilateral renal cortical necrosis, a bulky left rectus abdominis muscle with an intramuscular haematoma and active bleeding, and a bulky uterus. In the ICU she was intubated electively. Empirical tigecycline was added. Her HB- 8.2, Fibrinogen – 108, platelets – 27000. Gynecologist and Surgeon were involved, and the plan was to manage the haematoma conservatively by stabilizing coagulopathy with blood products and to reassess it later. All her blood counts were monitored regularly and were corrected with PRBC, FFP, Cryo and Single donor platelets. In view of acute kidney injury with oliguria and refractory metabolic acidosis, the first session of hemodialysis was performed on 06/02/2026. She also, during this initial course of stabilization, developed severe left‑ventricular dysfunction probably secondary to stress cardiomyopathy. Her FiO₂ requirement increased gradually, and lung ultrasonography showed features of ARDS. Her shock worsened, requiring very high dual inotropic support. Repeating ultrasound later showed no increase in the size of the haematoma. The patient had severe sepsis with multiorgan dysfunction and refractory shock. Shock was refractory for more than 24 hours with high FiO2 requirement. Her peripherals were cold and cyanotic. Hematologist, gastroenterologist, obstetrician‑gynaecologist, cardiologist, and nephrologist were involved in the care. Gradually the patient’s haemodynamics improved; dual inotropic support was tapered and stopped, and the FiO₂ requirement fell. Blood cultures grew in Serratia; Meropenem continued. Empirical teicoplanin was added later. She required regular haemodialysis. Distal gangrene of the upper and lower limbs, more on the right side, was noted, probably secondary to severe shock and inotropes. All counts stabilized and coagulopathy improved. With continued treatment the patient gradually improved but continued to have poor sensorium. EEG showed diffuse cerebral dysfunction. MRI of the brain showed hypoxic‑ischemic encephalopathy. A neurologist was involved.
Caretakers were communicated about the disease and the clinical condition, the poor prognosis and the poor chances of neuro recovery and prolonged hospitalization. The patient had persistently low fio2 requirements and in view of need for prolonged ventilation, tracheostomy was performed. Subsequent chest x-ray showed left lower lobe consolidation. Gradually the Fio2 requirement increased overnight. Morning lung scan showed lower lobe pneumonia with pneumothorax in upper lobe. The left side ICD was placed. Post ICD x-ray chest showed left lung near total consolidation. Empirical Aztreonem/Avibactam was started. The patient rapidly deteriorated by developing shock and with increasing Fio2. Her inotrope and Fio2 requirement increased rapidly with refractory shock. The patient had cardiac arrest, and resuscitation was initiated according to ACLS guidelines. Despite aggressive resuscitative measures, the patient succumbed to her illness and was declared dead.
Outcome: She ultimately succumbed to the illness on 20/02/2026
Cause of Death
Immediate cause
- Refractory shock
- Multiorgan dysfunction syndrome.
Antecedent cause: Pneumonia
Underlying cause
- Recent post sterilization status
- Sepsis of unknown origin with multiorgan dysfunction.
Nursing Management
Nursing management played a crucial role in the successful outcome of this patient with the coolant poisoning. Continuous assessment, early detection of complications and supportive care were essential throughout the treatment period.
Initial Assessment and Monitoring
- Conducted rapid assessment of airway breathing and circulation
- Monitored vital signs hourly
- Assessed level of consciousness hourly
- Preparation for intubation.
Ventilator Management
- Ensured airway patency and positioned the patient to prevent aspiration
- Observing for ventilator associated complications
- Regular suctioning using aseptic technique
- Monitoring arterial blood gas reports.
Circulatory Support and Fluid Management
- Established and maintained intravenous access
- Administered intravenous fluids as ordered to maintain adequate hydration
- Monitored blood pressure for hypotension
- Maintained strict intake and output chart hourly.
Tracheostomy care
- Sterile dressing changes
- Airway patency maintenance
- Humidification support
- Monitoring for infection, bleeding and tube obstruction.
Infection prevention
- Strict hand hygiene
- Barrier Nursing
- Monitoring temperature trends
- Early detection of sepsis indicators
- Followed a strict aseptic technique during all invasive procedures
- Provided regular oral care and skin care
- Monitored insertion site for signs of infection.
Hemodynamic Monitoring
- Continuous blood pressure monitoring
- Maintained strict intake and output chart hourly.
- Fluid balance assessment
- Early recognition of shock.
Psychological Support and Counselling
- Provided emotional support to the patient family.
- Encouraged expression of feelings and concerns
- Regular updates of family members.
Documentation
- Time based charting
- Ventilator monitoring records
- Medication administration records
- Critical event reporting.
Discussion
The patient developed severe sepsis post sterilization, leading to multiorgan dysfunction. Despite intensive care, she succumbed to complications. This case highlights the need for vigilant post- operative monitoring and timely sepsis management in high-risk patients.
Conclusion
This case highlights the unpredictable and potentially fatal deterioration that can occur even after an elective surgical procedure such as sterilization. The patient initially underwent sterilization at an outside hospital and later developed fever and respiratory distress, which required referral to a higher center for advanced critical care management. Despite aggressive treatment including mechanical ventilation, tracheostomy and continuous intensive monitoring the patient’s condition progressively worsened and resulted in death. An important aspect in this case was the history of self-medication for abortion taken one month prior to sterilization, which emphasizes the need for thorough history taking and clinical assessment before any elective procedures. Although the sterilization was performed later as a routine procedure, detailed evaluation of prior medical history remains essential to ensure patient safety. This report also highlights the need for awareness regarding the risk associated with self-medication practices. The public should be encouraged to seek proper medical consultation for health concerns rather than relying on unsupervised medications.